|
Part 1.
|
Orientation: What Is Old, and What Is New
|
|
Part 2.
|
Some Key Facts about Xrays and Ionizing Radiation in General
|
|
Part 3.
|
No Doubt about Benefits from Medical Radiation
|
|
Part 4.
|
Role of Medical Radiation in Causing Cancer and IHD,
Past and Present
|
|
Part 5.
|
Our Method for Calculating Fractional Causation
|
|
Part 6.
|
Eight Features Which Confer High Credibility on the Findings
|
|
Part 7.
|
Our Unified Model of Atherogenesis, and NonXray Co-Actors in IHD
|
|
Part 8.
|
A Personal Word: The Xray Deserves Its Honored Place in Health
|
|
Part 9.
|
Every Benefit of Medical Radiation: Same Procedures, Lower Dose-Levels
|
|
Part 10.
|
An Immense Opportunity: All Benefit, No Risk
|
Boxes, Figures, and Tables, in that (alphabetical) order, are located
in this book at the ends of the corresponding chapters.
|
|
Box 1.
|
Final Summary for Fractional Causation, by Medical Radiation, of Cancer and IHD.
|
|
Box 2.
|
Comparison of Dose-Response at Mid-Century: NonCancer NonIHD, Cancer, IHD.
|
|
Box 3.
|
Known Procedures Which Reduce Dosage from Medical Xrays.
|
|
Figure 1-A:
|
All-Cancers-Combined: Dose-Response between PhysPop and MortRates.
|
|
Figure 1-B:
|
Ischemic Heart Disease: Dose-Response between PhysPop and MortRates.
|
|
Figure 1-C:
|
NonCancer NonIHD Deaths: Dose-Response between PhysPop and MortRates.
|
 Part 1. Orientation: What Is Old, and What Is New
Part 1. Orientation: What Is Old, and What Is New
The
evidence presented in this book strongly indicates that
over 50% of the death-rate from Cancer today, and over 60%
of the death-rate from Ischemic Heart Disease today, are
xray-induced as defined and explained in Part 5 of the
Introduction. The finding means that xrays (including
fluoroscopy and CT scans) have become a necessary co-actor
--- but not the only necessary co-actor --- in causing most
of the death-rate from Cancer and from Ischemic Heart
Disease (also called Coronary Heart Disease, and Coronary
Artery Disease). In multi-cause diseases such as Cancer
and Ischemic Heart Disease, more than one necessary co-actor
per fatal case is very likely. Absence of any necessary
co-actor, by definition, prevents such cases. The concept
of xray-induced cases means cases which would be absent in
the absence of exposure to xrays.
Xrays
and other classes of ionizing radiation have been, for
decades, a proven cause of virtually all types of mutations ---
especially structural chromosomal mutations (such as deletions,
translocations, and rings), for which the doubling dose by xrays
is extremely low. Additionally, xrays are an established cause
of genomic instability, often a characteristic of the most
aggressive Cancers.
Not
surprisingly, a host of epidemiologic studies have firmly
established that xrays and other classes of ionizing radiation
are a cause of most varieties of human Cancer. This monograph
presents (a) the first compelling evidence that xrays are a
cause also of Ischemic Heart Disease (IHD) --- a very important
cause --- and presents (b) a Unified Model of Atherogenesis and
Acute IHD Events (Part 7 of this chapter).
We
have a high level of confidence that our findings, about the
important causal role of medical radiation in both Cancer and
IHD, are correct. Part 6 of this chapter identifies the
features of the work which produce this confidence.
Part 9 of this chapter points to demonstrations, by others, of
proven ways to reduce dose-levels of nontherapeutic medical
radiation by 50% or considerably more, without eliminating a
single diagnostic or interventional radiologic procedure and
without degrading the information provided by medical
radiation.
Reduction
of exposure to medical radiation can and will reduce
mortality rates --- from Cancer with certainty, and with very
great probability from Ischemic Heart Disease too.
 Part
2. Some Key Facts about Xrays and Ionizing Radiation in General
Part
2. Some Key Facts about Xrays and Ionizing Radiation in General
Most
physicians and other people appreciate the imaging
capability of the xray, but --- through no fault of their own
--- they are taught very little about the biological action of
those xrays which never reach the film or other image-receptor.
Part 2 provides some information about xrays and ionizing
radiation in general. These facts are well supported in the
peer-reviewed biomedical literature, in our text, and in our
Reference List.
2a. Capacity
to Commit Mayhem among the Genetic Molecules
The
biological damage from a medical xray procedure does not
come directly from the xray photons. The damage comes from
electrons, which those photons "kick" out of their normal atomic
orbits within human tissues. Endowed with biologically
unnatural energy by the photons, such electrons leave their
atomic orbits and travel with high speed and high energy through
their "home cells and neighboring cells. Each such electron
gradually slows down, as it unloads portions of its biologically
unnatural energy, at irregular intervals, onto various
biological molecules along its primary track (path).
The
molecular victims include, of course, chromosomal DNA, and
the structural proteins of chromosomes, and water. Even though
each energy-deposit transfers only a portion of the total energy
of a high-speed high-energy electron, the single deposits very
often have energies far exceeding any energy-transfer which
occurs in a natural biochemical reaction. Such energy-deposits
are more like grenades and small bombs
(Chapter 2,
Part 4a).
None of this is in dispute.
2b. The
Free-Radical Fallacy
There
is no doubt that, along the path of each high-speed
high-energy electron described above, the energy-deposits
produce various species of free radicals. Nonetheless, it is a
demonstrated fallacy (Appendix-C) to assume equivalence between
the biological potency of xrays and the biological potency of
the free radicals which are routinely produced by a cell's own
natural metabolism.
The
uniquely violent and concentrated energy-transfers,
resulting from xrays, are simply absent in a cell's natural
biochemistry. As a result of these "grenades" and "small
bombs," both strands of opposing DNA can experience a level of
mayhem far exceeding the damage which metabolic free-radicals
(and most other chemical species) generally inflict upon a
comparable segment of the DNA double helix.
2c. Ionizing
Radiation: A Uniquely Potent Mutagen
The
extra level of mayhem is what makes xrays (and other types
of ionizing radiation) uniquely potent mutagens. Cells can not
correctly repair every type of complex genetic damage, induced
by ionizing radiation, and sometimes cells can not repair such
damage at all (evidence discussed in Appendix-B and
Appendix-C). Not all mutated cells die, of course. If they all
died, there would be very little Cancer and no inherited
afflictions. Indeed, certain mutations confer a proliferative
advantage on the mutated cells. Exposure to xrays is a proven
cause of genomic instability --- a characteristic of many of the
most aggressive Cancers (Chapter 2,
Part 4b, and Appendix-D).
Unlike
some other mutagens, xrays have access to the genetic
molecules of every internal organ, if the organ is within the
xray beam. Within such organs, even a single high-speed
high-energy electron, set into motion by an xray photon, has a
chance (far from a certainty) of inducing the types of damage
which defy repair. That is why there is no risk-free (no safe)
dose-level (Appendix-B).
There
is widespread agreement that, by its very nature, ionizing
radiation at any dose-level can induce particularly complex
injuries to the genetic molecules. There is growing mainstream
acknowledgment that cellular repair processes are fallible, or
entirely absent, for various complex injuries to the genetic
molecules (Appendix-B and Appendix-C).
2d. The
Very Low Doubling-Dose for Xray-Induced Chromosomal
Mutations
The
inability of human cells, to repair correctly every type of
radiation-induced chromosomal damage, has been demonstrated in
nuclear workers (who received their extra low-dose radiation at
minimal dose-rates) and in numerous studies of xray-irradiated
human cells at low doses. Besides demonstrating non-repair or
imperfect repair, such studies have established that xrays have
an extremely low doubling-dose for structural chromosomal
mutations. (The doubling dose of an effect is the dose which
adds a frequency equal to the pre-existing frequency of that
effect.)
For
instance, the doubling-dose for the dicentric mutation is in
the dose range delivered by some common xray procedures, such as
CT scans and fluoroscopy --- i.e., in the dose range of 2 to 20
rads (references in Chapter 2,
Part 4b). The rad is a dose-unit
which is identical to the centi-gray (Appendix-A). We, and many
others, prefer the simpler name: Rad.
Xrays
are capable of causing virtually every known kind of
mutation --- from the very common types to the very complex
types, from deletions of single nucleotides, to chromosomal
deletions of every size and position, and chromosomal
re-arrangements of every type. When such mutations are not
cell-lethal, they endure and accumulate with each additional
exposure to xrays or other ionizing radiation
(Chapter 2,
Part 8c; and Appendix-B, Part 2d).
2e. Medical
Xrays as a Proven Cause of Human Cancer
Ionizing
radiation is firmly established by epidemiologic
evidence as a proven cause of almost every major type of human
Cancer (Chapter 2,
Part 4c).
Some of the strongest evidence
comes from the study of medical patients exposed to xrays ---
even at minimal dose-levels per exposure (Appendix-B, Part 2d).
Mounting mainstream evidence indicates that medical xrays are 2
to 4 times more mutagenic than high-energy beta and gamma rays,
per rad of exposure (Chapter 2, Part 7).
 Part
3. No Doubt about Benefits from Medical Radiation
Part
3. No Doubt about Benefits from Medical Radiation
Radiation
was introduced into medicine almost immediately after
discovery of the xray (by Wilhelm Roentgen) in 1895.
There
is simply no doubt that the use of radiation in medicine
has many benefits. The findings in this book provide no
argument against medical radiation. The findings do provide a
powerful argument for acquiring all the benefits of medical
radiation with the use of much lower doses of radiation, in both
diagnostic and interventional radiology. (Interventional
radiology refers primarily, but not exclusively, to the use of
fluoroscopy to acquire information during surgery and during
placement of catheters, needles, and other devices.)
Within
the professions of radiology and radiologic physics,
there are mainstream experts who have shown how the dosage of
xrays in current practice could be cut by 50%, or by
considerably more, in diagnostic and interventional radiology
--- without any loss of information and without eliminating a
single procedure (discussion in Part 9,
below). Among the current leaders in dose-reduction education are
Joel Gray, Ph.D. (recently retired from the Mayo Clinic's Department of
Radiology in Rochester, Minnesota) and Fred Mettler, M.D. (Chief
of Radiology, University of New Mexico School of Medicine in
Albuquerque, New Mexico).
 Part
4. Role of Medical Radiation in Causing Cancer and IHD, Past and Present
Part
4. Role of Medical Radiation in Causing Cancer and IHD, Past and Present
This
monograph has produced evidence with regard to two
hypotheses.
 Hypothesis-1: Medical radiation is a highly important
cause (probably the principal cause) of cancer mortality in the
United States during the Twentieth Century. Medical radiation
means, primarily but not exclusively, exposure by xrays ---
including fluoroscopy and CT scans. (Hypothesis-1 is about
causation of Cancer, so it is silent about radiation-therapy
used after a Cancer has been diagnosed.)
Hypothesis-1: Medical radiation is a highly important
cause (probably the principal cause) of cancer mortality in the
United States during the Twentieth Century. Medical radiation
means, primarily but not exclusively, exposure by xrays ---
including fluoroscopy and CT scans. (Hypothesis-1 is about
causation of Cancer, so it is silent about radiation-therapy
used after a Cancer has been diagnosed.)
 Hypothesis-2: Medical radiation, received even at very
low and moderate doses, is an important cause of death from
Ischemic Heart Disease (IHD); the probable mechanism is
radiation-induced mutations in the coronary arteries, resulting
in dysfunctional clones (mini-tumors) of smooth muscle cells.
(The kinds of damage to the heart and its vessels, observed from
very high-dose radiation and reported for decades, seldom
resemble the lesions of IHD --- details in Appendix J.)
Hypothesis-2: Medical radiation, received even at very
low and moderate doses, is an important cause of death from
Ischemic Heart Disease (IHD); the probable mechanism is
radiation-induced mutations in the coronary arteries, resulting
in dysfunctional clones (mini-tumors) of smooth muscle cells.
(The kinds of damage to the heart and its vessels, observed from
very high-dose radiation and reported for decades, seldom
resemble the lesions of IHD --- details in Appendix J.)
4a. These
Hypotheses in Terms of Multi-Cause Diseases
Cancer
and Ischemic Heart Disease are well established as
multi-cause diseases. The concept, that more than one necessary
co-actor is required per case, has already been discussed in
Parts 4 and 5 of the Introduction. In efforts to prevent these
multi-cause diseases, reduction or removal of any necessary
co-actor is a central goal. The evidence in this book is that
medical radiation has become a necessary co-actor in a high
fraction of the U.S. mortality rates from both diseases.
Fortunately, dosage from medical radiation is demonstrably
reducible without eliminating a single procedure.
4b. Fractional
Causation: Percentage of Death-Rates due to Medical Radiation
The
tabulation below shows the percentages, of the age-adjusted
death rates (m=male, f=female) from Cancer and IHD, due to
medical radiation at mid-century and at the most recent year for
which we have data. Box 1 at the end of this
chapter shows percentages for several specific types of
Cancer. Percentages for each intervening decade are shown in
the appropriate chapters and assembled in Chapter 66.
When
an entry of ~ 100% occurs, such a finding is fully
consistent with the fact that these diseases occurred before the
introduction of radiation into medicine, over a century ago.
Other mutagens (including radiation exposure from nature itself)
have been operative both before and after the introduction of
medical radiation. A finding, of about 100% of the death-rate
due to medical radiation in 1940, means that by 1940, a very low
fraction of such deaths would have occurred without medical
radiation as a co-actor.
Year Percent Year Percent
 All-Cancers-Combined, m 1940 90% 1988 74%
All-Cancers-Combined, m 1940 90% 1988 74%
 All-Cancers-Combined, f 1940 58% 1988 50%
All-Cancers-Combined, f 1940 58% 1988 50%
 Breast Cancer, f 1940 ~ 100% 1990 83%
Breast Cancer, f 1940 ~ 100% 1990 83%
 All-Cancer-Except-Genital, f 1940 75% 1980 66%
All-Cancer-Except-Genital, f 1940 75% 1980 66%
 Ischemic Heart Disease, m 1950 79% 1993 63%
Ischemic Heart Disease, m 1950 79% 1993 63%
 Ischemic Heart Disease, f 1950 97% 1993 78%
Ischemic Heart Disease, f 1950 97% 1993 78%
The
growing impact of cigarette smoking (Chapters 48, 49) almost
certainly explains why the shares from medical radiation in
1980-1993 are somewhat lower than in 1940-1950.
A
percentage such as 90% due to medical radiation (Fractional
Causation by medical radiation = 0.90) means that about 90% of
the death-rate would have been absent in the absence of medical
radiation. Circumstantial evidence is strong that nonxray
agents also were necessary co-actors in these same deaths.
Thus, Fractional Causation of 90% by medical radiation certainly
does not leave "just 10%" for all other causes combined, as
already illustrated in Part 5
of the Introduction.
Fractional
Causation, of a year-specific mortality rate
(MortRate) by medical radiation, refers to whatever rate occurs
in that year, and says nothing about whether the MortRate has
been rising or falling over time. Indeed, changes over time, in
the types and concentrations of non-xray co-actors to which
populations are exposed, can cause cancer MortRates
simultaneously to rise for some organs, fall for other organs,
and remain constant for still other organs (discussion in
Chapter 67, Part 2).
The
results in this book amply support Hypothesis-1 and the
first part of Hypothesis-2. While the central estimates of
Fractional Causation are statistically the most likely to be
correct, of course the actual percentages could be either higher
or lower. We note that percentages very much lower than the
central estimates would support each hypothesis, too.
 Part
5. Our Method for Calculating Fractional Causation
Part
5. Our Method for Calculating Fractional Causation
When
increments, in the death-rate from a disease, are
proportional to increments in exposure to an identified cause, a
linear dose-response exists between the causal agent and
increments in the death-rate.
The
evidence in this monograph repeatedly reveals a positive and
tight linear dose-response, between dose from medical radiation
and mortality rates from Cancer (discussion in
Chapter 5,
Part 5d).
By "tight," we mean highly reliable (statistically). As
we will explain, no group in our database escapes entirely from
exposure to medical radiation. In order to estimate what the
cancer mortality rates would be in the absence of medical
radiation, we use the basic technique of linear regression
analysis (Part 5c, below). After that basic
step, it is not at all complicated to calculate Fractional
Causation due to medical radiation
(Part 5g, below).
5a. The
Database for Age-Adjusted Mortality Rates (MortRates)
We
acquired the age-adjusted cancer MortRates per 100,000
population in each of the Nine Census Divisions of the USA, from
1940 onward --- separately for males and females, and for all
races combined (no exclusions). Such data are published by the
U.S. Government (details in Chapter 4).
For most types of Cancer, our data end in 1988-1990 (some end in 1980).
Also
we acquired the comparable age-adjusted MortRates for All
NonCancer Causes of Death --- as well as for selected individual
causes (such as IHD, Stroke, Diabetes Mellitus, Influenza and
Pneumonia, Accidents, etc.) --- in each of the Nine Census
Divisions.
These
MortRates, by Census Divisions, are the dependent
variables (the responses) in our dose-response studies. Because
the MortRates are age-adjusted, the Census Divisions are matched
with each other for age.
5b. The
Database for Dose: Physicians per 100,000 Population
During
the 1985-1990 period, the number of diagnostic medical
xray examinations performed per year in the USA was
approximately 200 million, excluding 100 million dental xray
examinations and 6.8 million diagnostic nuclear medicine
examinations. The source of these estimates (the 1993 Report of
UNSCEAR, the United Nations Scientific Committee on Atomic
Radiation, p.229, p.275) warns that 200 million could be an
underestimate by up to sixty percent.
Not
only is the number of annual examinations quite uncertain,
but the average doses per examination --- in actual practice,
not measured with a dummy during ideal practice --- vary
sometimes by many-fold from one facility to another, even for
patients of the same size. The variation by facility has been
established by a few on-site surveys of selected facilities,
because measurement and recording of xray doses are not required
for actual procedures (Part 9, below).
Fluoroscopy
is a major source of xray dosage, because the xray
beam stays "on" during fluoroscopy. Such doses are rarely
measured. When fluoroscopic xrays are used during common
diagnostic examinations, the total dose delivered varies with
the operator. When fluoroscopic xrays are used during surgery
and other nondiagnostic procedures, the total dose delivered
varies both with the operator and the particular circumstances.
The
uncertain number of procedures and the very uncertain doses
per procedure combine to cause profound uncertainty about
current average per capita population dose from medical
radiation (Chapter 2,
Part 3). Dose estimates for
past decades are even more uncertain (Chapter 2,
Part 2).
An Additional Gap in Knowledge: Risk-per-Rad Estimates
In
most of the studies which produce estimates of cancer-risk
per rad of xray dose, it is far from certain which participants
received which xray doses over their lifetimes, because such
doses were neither measured nor recorded. When a few
participants are (unintentionally) assigned a wrong
dose-estimate, the error can substantially alter the resulting
risk-per-rad estimates. This contributes to the great
uncertainty about the true risk-per-rad from xrays
(Chapter 2,
Part 7c).
The uncertainty is no secret. For example, the fifth
Committee on the Biological Effects of Ionizing Radiation stated
in its 1990 report (National Academy Press, at pp.46-47): "A
number of low-dose studies have reported risks that are
substantially in excess of those estimated in the present report
... Although such studies do not provide sufficient statistical
precision to contribute to the risk estimation procedure per se,
they do raise legitimate questions about the validity of the
currently accepted estimates."
A Solution to These Gaps in Knowledge
Medical
radiation procedures are initiated by a physician, even
if someone else actually performs the procedure. It is very
reasonable to think that the more physicians there are per
100,000 population, the more radiation procedures per 100,000
population will be ordered. Thus, we arrive at the premise that
average radiation dose, received per capita of population in a
specific Census Division from medical procedures during a
specific year, is approximately proportional to the number of
physicians per 100,000 population in that same Census Division
during that same year.
This
common-sense premise is well supported in the 1988 and 1993
reports of the United Nations Scientific Committee on Atomic
Radiation (details in our Chapter 3,
Part 1a), and is supported
specifically for the USA by data in a 1989 report from the
National Council on Radiation Protection and Measurements
(details in Chapter 3, Part 1a).
"PhysPop" Values in the Nine Census Divisions, over Many Decades
We
use the abbreviation, "PhysPop,"
for the quantity "Physicians per 100,000 Population." A PhysPop
value of 134 means 134 Physicians per 100,000 population, for the
specified year and place.
PhysPop
values for various calendar years have been compiled and
published for each state by the American Medical Association
over many decades (details in Chapter 3).
It is a routine
matter to combine such data appropriately, in order to obtain
PhysPop values for the Nine Census Divisions (details in Chapter
3). Because substantial differences in PhysPop values exist
among the Nine Census Divisions, it has been possible for us to
do dose-response studies, with PhysPop values in each Census
Division as surrogates for average per capita dose from medical
radiation in each corresponding Census Division.
Of
course, dose is cumulative (i.e., radiation-induced mutations
are cumulative). Moreover, in a population of mixed ages
(newborn to very advanced ages), the cancer-response to ionizing
radiation is spread out over at least four to five decades
(Chapter 2,
Part 8). Thus,
the age-adjusted cancer MortRates in
any single year --- say 1990 --- incorporate cases which are due
to radiation received in 1940, 1950, 1960, 1970, etc. It happens
that, during the 1921-1990 period, the rank order of the Census
Divisions --- by the size of their PhysPop values --- has been
remarkably stable (details in Chapter 3,
Box 1; see also Chapter
47, Table 47-A). Thus, PhysPop values are well-suited to be
surrogates for the relative size of average accumulated per
capita dose from medical radiation, among the Nine Census
Divisions.
5c. Illustrative
Regression (Input and Output), for All Cancers Combined
Linear
regression analysis is a branch of mathematics which,
among other things, evaluates how well correlated are sets of
paired values. In our dose-response studies, there are always
nine pairs of values, because there are Nine Census Divisions
--- each having its own age-adjusted MortRate (the y-variable)
and its own PhysPop value (the x-variable). On the lefthand side
of the next page, we show the input data for a regression whose
output is shown on the righthand side.
In
the output, two quantities measure the goodness (strength) of
the correlation: The R-squared value, and the ratio of the
X-coefficient divided by its Standard Error (X-Coef/S.E.).
 An R-squared value of 1.00 is perfection. An R-squared value
of 0.70 is very good. Those who are familiar with the
correlation coefficient, R, will recognize that R-squared values
are lower than the corresponding R-values (for instance, when R
= 0.83666, R-squared = 0.70; when R = 0.94868, R-squared =
0.90).
An R-squared value of 1.00 is perfection. An R-squared value
of 0.70 is very good. Those who are familiar with the
correlation coefficient, R, will recognize that R-squared values
are lower than the corresponding R-values (for instance, when R
= 0.83666, R-squared = 0.70; when R = 0.94868, R-squared =
0.90).
 A ratio of (X-Coef/S.E.) of about 2.0 generally indicates a
statistically significant correlation. A ratio of 4.0 is a
tight correlation. A ratio above 4.0 is very tight. The ratio
describes the reliability of the slope in a line of best fit.
A ratio of (X-Coef/S.E.) of about 2.0 generally indicates a
statistically significant correlation. A ratio of 4.0 is a
tight correlation. A ratio above 4.0 is very tight. The ratio
describes the reliability of the slope in a line of best fit.
In
Part 5d, the male 1940 MortRates per 100,000 population, for
All-Cancers-Combined, are regressed upon the 1940 PhysPop values
(which represent accumulated doses from earlier years of medical
radiation). The regression reveals a spectacularly tight
correlation: R-squared = 0.9508.
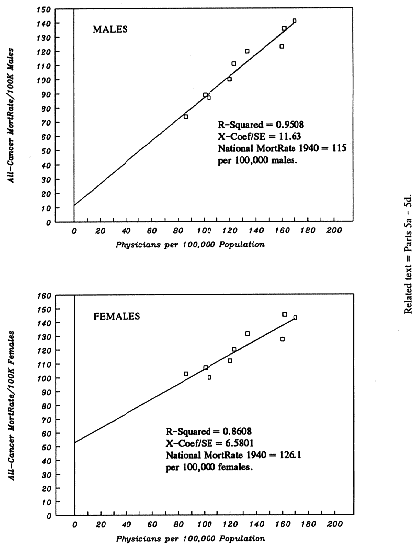
5d. Figure
1-A: Graph of the 1940 PhysPop-Cancer
Dose-Response (Males, Females)
The
regression output (below) provides all the information
necessary to calculate and to graph the line of best fit for the
nine pairs of real-world observations (listed below). Chapter
6, Part 3, shows how. The resulting graph is presented in the
upper half of Figure 1-A, at the end o
this chapter. The nine boxy symbols in Figure 1-A represent the
nine pairs of actual observations from the x,y columns below. For
example, the box farthest to the right represents the pair with
the highest PhysPop value: The Mid-Atlantic pair.
Figure
1-A also presents the comparable graph for females
(borrowed from Chapter 7). It was prepared after regressing the
female 1940 MortRates per 100,000 population, for
All-Cancers-Combined, upon the 1940 PhysPop values (which
represent accumulated doses from earlier years of medical
radiation).
5e. The
Dose-Response Findings for Specific Sets of Cancer
In
addition to All-Cancers, we examined the dose-response for
various sets of Cancers. With only one exception (female
Genital Cancers), all the regression analyses revealed strong
positive correlations between PhysPop and the 1940 Cancer
MortRates, by Census Divisions. A summary of their R-squared
values is in Column D of Box 1, after the text of this
chapter.
5f. NonCancer
Causes of Death: IHD Separates Itself from Other Causes
Before
exploring the post-1940 decades, we asked, "Do the same
strong positive correlations exist for noncancer causes of
death?
They
definitely do not. When we studied All Causes Except
Cancer (Chapter 24), we found a nonsignificant negative
relationship between PhysPop and MortRates. Curiosity drove us
also to study specific noncancer MortRates in 1940 versus
PhysPop. Almost all regression analyses revealed negative
relationships between PhysPop and noncancer MortRates. There is
a summary of those findings in the upper part of
Box 2, at the end of this chapter. A
negative X-coefficient means a downward slope.
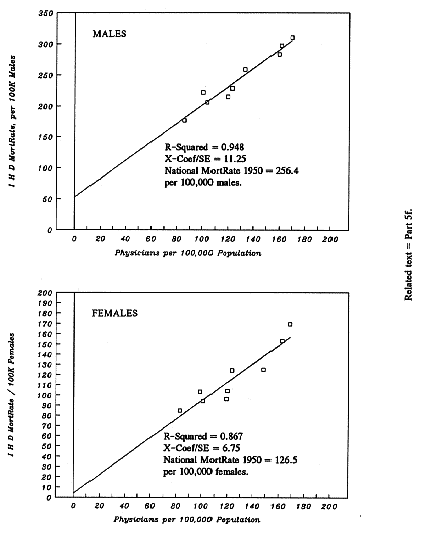
Strong positive Correlation between PhysPop and 1950 IHD MortRates
We
arrived late at regressing Ischemic Heart Disease (IHD)
MortRates on PhysPop, by Census Divisions, because there are no
MortRate data for IHD until 1950. When we finally regressed the
1950 MortRates for IHD on PhysPop, we were astonished by the
results (Chapters 40 and 41). What fell out of the data are
very strong positive correlations with PhysPop --- which are
graphed as Figure 1-B at the end of this chapter.
- Male IHD MortRates vs. PhysPop: R-sq = 0.95 and Xcoef/SE = 11.25.
- Female IHD MortRates vs. PhysPop: R-sq = 0.87 and Xcoef/SE = 6.75.
Such
spectacular correlations do not happen by accident. They
"demand" an explanation. The resemblance to the positive
dose-response for Cancer is self-evident. These two diseases
unambiguously sort themselves out from NonCancer NonIHD causes
of death, with respect to medical radiation (PhysPop). The
positive dose-response between PhysPop and Cancer is no
surprise, because xrays are a proven cause of Cancer. For IHD,
the findings above invoke the Law of Minimum Hypotheses:
Medical radiation is a cause of Ischemic Heart Disease, too.
Our Unified Model of Atherogenesis (Part 7,
below) proposes how radiation-induced dysfunctional
clones of smooth muscle cells, in the coronary arteries, may
interact with atherogenic lipoproteins to explain the strong
positive correlations presented above.
Strong negative Correlation
between PhysPop and 1950 NonCancer NonIHD MortRates
When
both Cancer and IHD are removed from Causes of Death, the
correlation between PhysPop and MortRates for the remaining
Causes of Death (NonCancer NonIHD) is not only negative, but it
also is statistically significant. That relationship is
depicted in Figure 1-C --- borrowed from Chapter 25. The
contrast is dramatic, between Figure 1-C and the two preceding
figures. Box 2, at the end of this chapter, presents the
findings for specific NonCancer Non IHD causes of death.
5g. From
Positive Dose-Response to Fractional Causation: The Calculation
The
observed PhysPop values and the observed MortRates, by
Census Divisions, reveal a positive, linear dose-response of
great strength between medical radiation and the mid-century
MortRates for Cancer and (separately) for Ischemic Heart
Disease.
In
order to estimate what share of the National MortRates for
these diseases was due to medical radiation, we use the
regression output to identify what the MortRates for each
disease would have been at that time, if the population had
received no medical radiation. The Constant is the value of the
y-variable (the MortRate) when the x-variable (PhysPop) is
zero. Obviously, if there had been no physicians per 100,000
population, there would have been no medical radiation. On our
graphs, the Constant is the value of y where the line of best
fit intercepts the vertical y-axis.
Example
from Part 5d, above: In the regression output, the
Constant = 11.5 --- matching the y-intercept in the upper graph of
Figure 1-A. From Chapter 6, Table 6-B, we have
the datum that the 1940 national age-adjusted male MortRate
from All Cancers Combined was 115.0 fatal Cancers per 100,000 male
population. Of these 115.0 cases, only 11.5 cases would have
occurred if there had been no medical radiation. The number of
fatal cases (per 100,000 population) in which medical radiation
was a required co-actor was (115.0 minus 11.5), or 103.5 cases.
And the Fractional Causation by medical radiation was 103.5 /
115.0, or 0.90 --- 90%.
This
is the manner in which Fractional Causation by medical
radiation is estimated, both for Cancer and for IHD MortRates,
throughout this book. For the decades beyond mid-century, one
adjustment was required (and executed in plain view) for the
impact of cigarette smoking, an important co-actor whose
intensity was not matched across the Nine Census Divisions
(Chapter 48).
Returning
to the example from Part 5d, we want to estimate
the Upper and Lower 90% Confidence Limits on the Fractional
Causation by medical radiation of the male 1940 National
All-Cancer MortRate. These limits are, respectively, 99% and
75%. These limits are derived from the reliability of the slope
of the line of best fit, because its slope (the X-coefficient)
determines the value of the y-intercept (the Constant). The
regression output in Part 5d provides the required values: The
X-coefficient is 0.7557 units of y per unit of x, with a
Standard Error of 0.0650. Calculation of the Confidence Limits
is first demonstrated in Chapter 6, Part 4.
 Part
6. Eight Features Which Confer High Credibility on the Findings
Part
6. Eight Features Which Confer High Credibility on the Findings
This
monograph presents evidence that medical radiation is an
important cause of both fatal Cancer and fatal Ischemic Heart
Disease in the USA. There are eight features of our findings
which endow us with high confidence that the findings are
correct, and so we call those features to the attention of
readers:
 First, the findings occur from data which were collected long
ago for other purposes --- namely the collection of Vital
Statistics from each state on the causes of death per 100,000
population, and the collection of information from each state on
the number of physicians per 100,000 population (PhysPop
values). Thus, these databases are free from any conceivable
bias with respect to Hypothesis-1 or Hypothesis-2. This is no
small matter. The first obligation of objective analysts is to
be able to assure themselves and the public that the raw data
which they employ are trustworthy and neutral with respect to
the topic.
First, the findings occur from data which were collected long
ago for other purposes --- namely the collection of Vital
Statistics from each state on the causes of death per 100,000
population, and the collection of information from each state on
the number of physicians per 100,000 population (PhysPop
values). Thus, these databases are free from any conceivable
bias with respect to Hypothesis-1 or Hypothesis-2. This is no
small matter. The first obligation of objective analysts is to
be able to assure themselves and the public that the raw data
which they employ are trustworthy and neutral with respect to
the topic.
 Second, the findings occur from an enormous database: The
entire U.S. population. (132 million in 1940; 247 million in
1990). It is hard to imagine a larger prospective study than one
which "enrolls" the entire U.S. population in its nine
dose-cohorts (Chapter 22, Part 4). All other things being
equal, the larger the database, the more reliable are the
results.
Second, the findings occur from an enormous database: The
entire U.S. population. (132 million in 1940; 247 million in
1990). It is hard to imagine a larger prospective study than one
which "enrolls" the entire U.S. population in its nine
dose-cohorts (Chapter 22, Part 4). All other things being
equal, the larger the database, the more reliable are the
results.
 Third, the findings occur without dependence on permanently
uncertain dose-estimates in medical rads and without dependence
on unsettled estimates of cancer-risk per medical rad
(Part 5b,
above). Instead, the relative sizes of medical doses,
proportional to PhysPop values in the Nine Census Divisions,
directly reveal the magnitude of Fractional Causation, by
medical radiation, of the death-rates from Cancer and from
Ischemic Heart Disease. This aspect of the method itself is a
source of enormous credibility for the results.
Third, the findings occur without dependence on permanently
uncertain dose-estimates in medical rads and without dependence
on unsettled estimates of cancer-risk per medical rad
(Part 5b,
above). Instead, the relative sizes of medical doses,
proportional to PhysPop values in the Nine Census Divisions,
directly reveal the magnitude of Fractional Causation, by
medical radiation, of the death-rates from Cancer and from
Ischemic Heart Disease. This aspect of the method itself is a
source of enormous credibility for the results.
 Fourth, the findings are not the product of elaborate
statistical manuevers and adjustments occurring, beyond
realistic review, in a computer. While statistical operations
are an essential part of epidemiology, we regard findings in the
biomedical literature as unreliable, if they are the product of
layer upon layer of such operations. In this monograph, we have
confined ourselves to one layer of statistical operation: The
basic linear regression with just one independent variable.
(Every step in our findings --- from the raw data to the
estimated values of Fractional Causation by medical radiation
--- has been presented in the open.)
Fourth, the findings are not the product of elaborate
statistical manuevers and adjustments occurring, beyond
realistic review, in a computer. While statistical operations
are an essential part of epidemiology, we regard findings in the
biomedical literature as unreliable, if they are the product of
layer upon layer of such operations. In this monograph, we have
confined ourselves to one layer of statistical operation: The
basic linear regression with just one independent variable.
(Every step in our findings --- from the raw data to the
estimated values of Fractional Causation by medical radiation
--- has been presented in the open.)
 Fifth, the mid-century dose-responses between PhysPop and the
MortRates for Cancer and for Ischemic Heart Disease are
extremely strong. There is nothing marginal about the
findings. They are almost spectacular in their strength. Even
without linear regression, it would be clear from Figures
1-A and 1-B
that the nine real-world observations (the boxy symbols)
cluster very closely around a straight and upward line. The
nearly perfect correlations provide a solid foundation for
confidence in the resulting estimates of Fractional Causation by
medical radiation, both for Cancer and for Ischemic Heart
Disease.
Fifth, the mid-century dose-responses between PhysPop and the
MortRates for Cancer and for Ischemic Heart Disease are
extremely strong. There is nothing marginal about the
findings. They are almost spectacular in their strength. Even
without linear regression, it would be clear from Figures
1-A and 1-B
that the nine real-world observations (the boxy symbols)
cluster very closely around a straight and upward line. The
nearly perfect correlations provide a solid foundation for
confidence in the resulting estimates of Fractional Causation by
medical radiation, both for Cancer and for Ischemic Heart
Disease.
 Sixth, MortRates from diseases in general very definitely do
not share a strong positive correlation with PhysPop values. On
the contrary. PhysPop discriminates among diseases. Figure
1-C displays the significant negative correlation between
PhysPop and all NonCancer NonIHD Causes of Death at mid-century
--- and the negative correlation persists through subsequent
decades (Chapter 25, Box 1).
Sixth, MortRates from diseases in general very definitely do
not share a strong positive correlation with PhysPop values. On
the contrary. PhysPop discriminates among diseases. Figure
1-C displays the significant negative correlation between
PhysPop and all NonCancer NonIHD Causes of Death at mid-century
--- and the negative correlation persists through subsequent
decades (Chapter 25, Box 1).
Box
2 summarizes the findings for specific as well as combined
NonCancer NonIHD Causes of Death, and contrasts them with the
findings for All-Cancers, specific Cancers, and IHD.
A
mountain of powerful evidence is summarized on that single
page. The real-world observations clearly show that Cancer and
Ischemic Heart Disease belong together, and not with the other
diseases, with respect to PhysPop. These observations "demand"
an explanation, which is supplied by the proportionality between
PhysPop and average accumulated per capita dose from medical
radiation.
Figure
1-A has a ready explanation, based on two undisputed
facts: 1) Physicians cause exposure to medical radiation, and
2) Radiation is a proven cause of
Cancer. Figure 1-B
also has an explanation which is tied to real-world evidence: 1)
Physicians cause exposure to medical radiation; 2) Radiation is
a proven cause of mutations of virtually every sort; and 3) Some
evidence exists, prior to this monograph, that acquired
mutations are co-actors in atherogenesis (Chapter 44, Parts 8
and 9). In contrast to the evidence-based explanations above,
various speculations are possible (Chapter 68). For example,
perhaps physicians do something additional (besides causing
exposure to radiation) which causes both Cancer and Ischemic
Heart Disease. If that speculation seems credible, then clearly
the National Institutes of Health should give top priority to
identifying what the physicians do.
 Seventh, the conclusion, that medical radiation is a major
cause of both fatal Cancer and fatal Ischemic Heart Disease,
very reasonably explains the tight positive correlations between
PhysPop and the MortRates for Cancer and for IHD (and the
absence of such correlations for NonCancer NonIHD MortRates),
while various alternative proposals fall short (Chapter 68).
Moreover, the conclusion does not produce conflicts with
well-established facts (Introduction, and Chapters 46 and 67).
Indeed, the conclusion helps to explain some of them (Chapter
46).
Seventh, the conclusion, that medical radiation is a major
cause of both fatal Cancer and fatal Ischemic Heart Disease,
very reasonably explains the tight positive correlations between
PhysPop and the MortRates for Cancer and for IHD (and the
absence of such correlations for NonCancer NonIHD MortRates),
while various alternative proposals fall short (Chapter 68).
Moreover, the conclusion does not produce conflicts with
well-established facts (Introduction, and Chapters 46 and 67).
Indeed, the conclusion helps to explain some of them (Chapter
46).
 Eighth, this monograph --- although employing completely
independent data and methods from our 1995/96 monograph about
Breast Cancer --- nonetheless produces remarkably similar
estimates of the Fractional Causation of recent Breast Cancer
rates by medical radiation (Chapter 67, Part 5c).
Eighth, this monograph --- although employing completely
independent data and methods from our 1995/96 monograph about
Breast Cancer --- nonetheless produces remarkably similar
estimates of the Fractional Causation of recent Breast Cancer
rates by medical radiation (Chapter 67, Part 5c).
 Part
7. Our Unified Model of Atherogenesis, and NonXray Co-Actors in IHD
Part
7. Our Unified Model of Atherogenesis, and NonXray Co-Actors in IHD
As
noted above, this monograph's real-world evidence clearly
shows that Cancer and Ischemic Heart Disease belong together,
and not with the other causes of death, with respect to
PhysPop. The positive dose-response between PhysPop and Cancer
is certainly not strange. Cancer is the single cause of death
already well-proven (prior to this monograph) to be inducible by
ionizing radiation --- and average population exposure to
ionizing radiation from medical procedures is approximately
proportional to PhysPop.
The
surprise is our unambiguous finding of a tight positive
correlation between PhysPop and IHD MortRates, a result which
indicates strongly that Ischemic Heart Disease also is inducible
by medical radiation. With respect to "surprise," a reminder is
appropriate: The kinds of damage to the heart and its vessels,
observed from very high-dose radiation and reported for decades,
seldom resemble the lesions of IHD --- details in Appendix-J.
Our
monograph is essentially the first, large prospective study
on induction of fatal Ischemic Heart Disease by medical
radiation. The results are stunning in their strength. Such
strong dose-response relationships do not occur by accident.
7a. Earl
Benditt's Work on Monoclonality in Atherosclerotic Plaques
We
might be less surprised, by the strong positive dose-response
between medical radiation and IHD MortRates, if we (and others)
had paid more attention to a different type of evidence,
available since 1973. We mean evidence supporting a role for
mutagens in atherosclerosis. Such evidence came into existence
at the University of Washington School of Medicine, Department
of Pathology, when Earl Benditt and colleagues found evidence of
monoclonality in atherosclerotic plaques in 1973 --- findings
which have been replicated several times (Chapter 44, Parts 8 +
9). The fact, that ionizing radiation is a uniquely potent
mutagen, provides the foundation for the second part of
Hypothesis-2 --- our Unified Model of Atherogenesis
(Part 7c, below).
7b. A
Reality-Check, for Consistency in Our Findings
Our
dose-response evidence, that medical radiation is an
important cause of both Cancer and Ischemic Heart Disease,
elicits a "prediction." The MortRates for the two diseases
should show a persistent positive correlation with each other,
by Census Divisions, over time --- and should simultaneously
show a distinctly different relationship with MortRates for
NonCancer NonIHD Causes of Death, which are not inducible by
ionizing radiation. The expectation is well met, as we show in
Appendix-N.
7c. Our
Unified Model of Atherogenesis and Acute IHD Events
Our
Unified Model of Atherogenesis and Acute IHD Events (Chapter
45) combines the evidence in this book, that medical radiation
has an important causal role in mortality from Ischemic Heart
Disease, with the abundant evidence elsewhere that certain
lipoproteins in the bloodstream also have an important causal
role in mortality from Ischemic Heart Disease (Chapter 44, Parts
3,4,5,6,7).
Our
view (shared by many others) is that the plasma lipoproteins
have no physiologic function in the intimal layer of the
coronary arteries, and that under normal circumstances, their
rate of entry and exit from the intimal layer is in balance. We
propose that what disrupts this lifelong egress of lipoproteins
from the intima --- with the disruption occurring only at
specific locations --- are mutations acquired from medical
radiation and from other mutagens.
In
our Unified Model, some mutations acquired by smooth muscle
cells render such cells dysfunctional and give such cells a
proliferative advantage --- so that they gradually replace
competent smooth muscle cells at a localized patch of artery (a
mini-tumor). And this patch of cells, unable to process
lipoproteins correctly, becomes the site of chronic
inflammation, resulting in construction of an atherosclerotic
plaque --- whose fibrous cap is sometimes too fragile to contain
the highly thrombogenic lipid-core within the plaque. The
Unified Model is described in more detail in Chapter 45. Then
Chapter 46 describes how the model helps to explain, or is
consistent with, established observations --- including the
existence of many additional co-actors in the causation of
mortality from Ischemic Heart Disease.
 Part
8. A Personal Word: The Xray Deserves Its Honored Place in Health
Part
8. A Personal Word: The Xray Deserves Its Honored Place in Health
The
finding, that radiation from medical procedures is a major
cause of both Cancer and Ischemic Heart Disease, does not argue
against the use of xrays, CT scans, fluoroscopy, and
radioisotopes in diagnostic and interventional radiology. Such
uses also make very positive contributions to health. We deeply
respect those contributions, and the men and women who achieve
them.
This
author is most definitely not "anti-xray" or
"radio-phobic." As a graduate student in physical chemistry, I
worked very intimately with radiation, in the quest for the
first three atomic-bombs. Subsequently, in medical school, I
considered becoming a radiologist. In the late 1940s, I did
nuclear medicine with patients having a variety of hematological
disorders. In the 1960s, I did chemical elemental analysis of
human blood by xray spectroscopy. In the early 1970s, our group
at the Livermore National Laboratory induced genomic instability
in human cells with gamma rays.
In
short, I fully appreciate the benefits and insights (in
medicine and other fields) which ionizing radiation makes
possible.
But
no one honors the xray by treating it casually or by failing
to acknowledge that it is a uniquely potent mutagen. One honors
the xray by taking it seriously. While doses from diagnostic
and interventional radiology are very low relative to doses used
for cancer therapy, diagnostic and interventional xray doses
today are far from negligible (some examples in
Chapter 2,
Part 7e). The
widely used CT scans, and the common diagnostic
examinations which use fluoroscopy, and interventional
fluoroscopy (e.g., during surgery), deliver some of the largest
nontherapeutic doses of xrays. In 1993, the United Nations
Scientific Committee on the Effects of Atomic Radiation warned,
appropriately, in its Annual Report:
"Although
the doses from diagnostic xray examinations are
generally relatively low, the magni- tude of the practice makes
for a significant radiological impact" (UNSCEAR 1993, p.228/40).
In the USA until about 1970, fetal irradiation occurred
during ~ 1 pregnancy per 14
Chapter 2,
Part 2d).
 Part 9.
Part 9.
|
Every Benefit of Medical Radiation:
Same Procedures, Lower Dose-Levels
|
The
fact that ionizing radiation is a uniquely potent mutagen,
and the finding that radiation from medical procedures is a
major cause of both Cancer and Ischemic Heart Disease, clearly
indicate that it would be appropriate in medicine to treat
dosage of ionizing radiation at least as carefully as we treat
dosage from potent medications. In the medical professions, we
do not administer unmeasured doses of powerful pharmaceuticals,
and we do not take a casual view of a 5-fold, 10-fold, even
20-fold elevation in dosage of such medications.
By
contrast, in both the past and the present, unmeasured doses
of xrays are the rule --- not the exception
(Chapter 2, Parts
2,
3a, and
3e).
When sampling has been done, in which actual
measurements are taken, dosage has been found to vary from one
facility to another by many-fold, for the same procedure for
patients of the same size. The reason for large variation is
obvious from the list of numerous proven ways to reduce dosage
(Box 3 at the end of this chapter). Facilities which apply all
the measures can readily achieve average doses more than 5-fold
lower than facilities which apply very few measures.
Certain Spinal Xrays: A Dramatic Demonstration
The
potential for dose-reduction may far exceed 5-fold for some
common xray exams. This has already been demonstrated for the
spinal xrays employed to monitor progress in treating idiopathic
adolescent scoliosis, a lateral curvature of the spine. An
estimated 5% of American children, or more, have this disorder.
In a most responsible way, Dr. Joel Gray and co-workers at the
Mayo Clinic developed radiologic techniques for scoliosis
monitoring which can reduce measured xray dose to various organs
as follows (Gray 1983 in J. of Bone & Joint Surgery 65-A:
5-12):
 Abdominal exposure: 8-fold reduction.
Abdominal exposure: 8-fold reduction.
 Thyroid exposure: 20-fold reduction (with a back to front
radiograph), and 100-fold reduction (with a lateral
radiograph).
Thyroid exposure: 20-fold reduction (with a back to front
radiograph), and 100-fold reduction (with a lateral
radiograph).
 Breasts: 69-fold reduction (with a back to front
radiograph), and 55-fold reduction (with a lateral radiograph).
Breasts: 69-fold reduction (with a back to front
radiograph), and 55-fold reduction (with a lateral radiograph).
They
report, "These reductions in exposure were obtained without
significant loss in the quality of the radiographs and in most
instances, with an improvement in the over-all quality of the
radiograph due to the more uniform exposure.
9a. Dose-Measurement:
Low Cost and High Importance
Incorporated
in Box 3's list, under the term "Quality
Assurance," is measurement of dose-levels. Only frequent
measurements can provide the feedback required to make continual
dose reductions --- and also to prevent continual dose
increments. The combination of frequent measurements, with an
enhanced recognition that each xray photon matters, can achieve
a very great deal all by themselves. Nearly everyone takes
pride in doing better and better. The evidence, that a series
of small improvements can amount to a big difference in result,
is abundant elsewhere in medicine and pharmacology.
Fortunately,
it is extremely easy to measure entrance-doses
during a radiation procedure. One just presses on a small
self-adhesive patch called a TLD (thermo-luminescent dosimeter),
which does not interfere at all with the procedure. Moreover,
the cost for a TLD, including its subsequent "reading," is just
a few dollars.
We
note that no major equipment purchases are required either to
achieve the benefits of quality control (an estimated 2-fold
reduction in average dose-level in radiography, Box 3) or to
achieve better operator-techniques in fluoroscopy (an estimated
2-to-10-fold reduction in dose, Box 3). Cost is not a big
obstacle to taking dose-reduction seriously. The big obstacle
is the recognition that it really matters.
Mammography: A Model of Success
The
importance of dose-reduction for the mammographic
examination has been recognized, and such doses have been
reduced by about a factor of ten in recent years. "Where there
is a will, there is a way." In certified mammography centers
today, doses are routinely verified periodically, and
measurements provide the feedback required, in order to achieve
constant dose-reduction instead of upward creep.
9b. The
Benefits of Every Procedure --- with Far Less Dose
Dose-reduction
can be a truly safe measure. It is clear that
average per patient doses from diagnostic and interventional
radiology could be reduced by a great deal without reducing the
medical benefits of the procedures in any way. We can summarize
from Box 3:
 Radiography: Quality-assurance (dose-reduction by an average
factor of 2), beam-collimation (by a factor up to 3), rare-earth
screens (by a factor of 2 to 4), rare-earth filtration (by a
factor of 2 to 4), use of carbon-fibre materials (by a factor of
2), gonadal shielding (by a factor of 2 to 10 for the gonads).
Radiography: Quality-assurance (dose-reduction by an average
factor of 2), beam-collimation (by a factor up to 3), rare-earth
screens (by a factor of 2 to 4), rare-earth filtration (by a
factor of 2 to 4), use of carbon-fibre materials (by a factor of
2), gonadal shielding (by a factor of 2 to 10 for the gonads).
 Digital Radiography: Decrease in contrast resolution, when
such resolution is not needed (dose-reduction by a factor of 2
to 3), use of a pulsed system (by a factor of 2).
Digital Radiography: Decrease in contrast resolution, when
such resolution is not needed (dose-reduction by a factor of 2
to 3), use of a pulsed system (by a factor of 2).
 Fluoroscopy: Changes in the operator's technique
(dose-reduction by a factor of 2 to 10), variable aperture iris
on TV camera (by a factor of 3), high and low dose-switching (by
a factor of 1.5), acoustic signal related to dose-rate (by a
factor of 1.3), use of a 105mm camera (by a factor of 4 to 5).
Additional methods not specified in the list: Use of a circular
beam-collimator when the image-receiver is circular
(Chapter 2,
Part 3d),
adoption of "freeze-frame" or "last-image-hold
capability, and restraint in recording fluoroscopic images
(Chapter 2, Part 3e).
Fluoroscopy: Changes in the operator's technique
(dose-reduction by a factor of 2 to 10), variable aperture iris
on TV camera (by a factor of 3), high and low dose-switching (by
a factor of 1.5), acoustic signal related to dose-rate (by a
factor of 1.3), use of a 105mm camera (by a factor of 4 to 5).
Additional methods not specified in the list: Use of a circular
beam-collimator when the image-receiver is circular
(Chapter 2,
Part 3d),
adoption of "freeze-frame" or "last-image-hold
capability, and restraint in recording fluoroscopic images
(Chapter 2, Part 3e).
 Part
10. An Immense Opportunity: All Benefit, No Risk
Part
10. An Immense Opportunity: All Benefit, No Risk
The
evidence in this monograph, on an age-adjusted basis, is
that most fatal cases of Cancer and Ischemic Heart Disease would
not happen as they do, in the absence of xray-induced
mutations. We look forward to responses to our findings.
We
have also presented findings, from outside sources, that
average per patient radiation doses from diagnostic and
interventional radiology could be reduced by a great deal,
without reducing the medical benefits of the procedures in any
way. The same procedures can be done at substantially lower
dose-levels (Part 9, above).
10a. Does
the Public Need a Denial, "For Its Own Good" ?
One
type of response to this monograph may be that the findings
need to be denied immediately (without examination), lest the
public refuse to accept the benefits of xray procedures.
This
type of response, insulting to the public, would not be
consistent with reality. In reality, the public accepts a host
of dangerous medications and procedures, in exchange for their
demonstrable benefits --- sometimes, for undemonstrated
benefits. Very few people will forego the obvious benefits from
diagnostic and interventional radiology, just because such
procedures confer a risk of subsequent Cancer and IHD. The only
change will probably be that people will demand that the same
degree of care, now exercised with respect to dosage of potent
medications, be exercised with respect to dosage of radiation
from each procedure. They will want to avoid a dose-level of,
say, ten rads --- if the same information could be acquired with
one rad. They do not deserve "one useful part of information,
and nine unnecessary parts of extra risk of Cancer and IHD."
Patients will want more measurements, and fewer assumptions,
about the doses delivered. But they will not reject the
procedures themselves.
10b. Do
Nothing Until the Work Is Independently Confirmed?
A
second response, to the evidence in this monograph, may be
that doses in diagnostic and interventional radiology should not
be reduced until our work is independently confirmed.
The
concept, "independent confirmation," is meaningless without
equally credible, but independent, sets of data. If one is
seriously interested in new prevention-measures for Cancer and
Ischemic Heart Disease, then one really needs to ask: Will it
ever be possible to conduct a more reliable evaluation --- of
Fractional Causation, by medical radiation, of Cancer and IHD
--- than the evaluation provided by the databases we used in
this book? We doubt it, for the reasons described in
Part 5b
above. As for replication of our results from the same
databases (PhysPops and age-adjusted MortRates, by Census
Divisions), that could be promptly achieved.
It
is worth emphasis that validity of the first part of
Hypothesis-2 (medical radiation is an important cause of IHD)
does not depend on the validity of the second part of
Hypothesis-2 (our Unified Model of Atherogenesis --- Part 7c,
above). The Unified Model will definitely need independent
testing. This might consume decades. Meanwhile, why deny
patients the benefits of eliminating uselessly high doses of
medical radiation?
10c. The
"Advocacy Issue" and the Hippocratic Oath
It
is very often said that, if scientists advocate any action
based on their findings, they undermine their scientific
credibility. If such scientists stand to benefit financially
from the actions they advocate, such suspicion occurs
naturally. But even in such circumstances, if their work is
presented in a way which anyone can replicate, it should be
impossible for their advocacy to diminish the scientific
credibility of their work.
Our
findings are not encumbered either by financial interests or
by any barriers to replication. We have high confidence in the
scientific credibility of the results, for the reasons presented
in Part 6. The findings stand on their own, whether or not we
advocate any action.
I
have spent a lifetime studying the causes of Ischemic Heart
Disease, and then Cancer, in order to help prevent such
diseases. So it would be pure hypocrisy for me to feign a lack
of interest in any preventive action which would be both safe
and benign. And when sources, completely independent from me,
set forth their findings that such action is readily feasible
--- namely, significant dose-reduction in diagnostic and
interventional radiology --- it would be worse than silly for me
to pretend that I have no idea what action should occur. After
all, as a physician, I took the Hippocratic Oath: "First, do no
harm." Silence would contribute to the harm of millions of
people.
10d. Why
Wait? What Is the Purpose?
Although
it is commonly assumed that radiation doses are
"negligible" from modern medical procedures, the assumption is
definitely mistaken. In reality, estimated dose-levels today
from some common xray procedures are far from negligible, as
illustrated in Chapter 2,
Part 7e. Both the downward and upward
forces upon post-1960 dose-levels are discussed in Chapter 2,
Part 3. The net result is unquantifiable.
An
estimated 35% to 50% of some higher-dose diagnostic
procedures are currently received by patients below age 45
(details in Chapter 2,
Part 3f) --- when the carcinogenic impact
per dose-unit is probably stronger than it is after age 65 or
so.
In
diagnostic and interventional radiology, dose-reduction would
be wholly safe, quite inexpensive, and guaranteed beneficial ---
because induction of Cancer by ionizing radiation has been an
established fact for decades. (The contribution of
radiation-induced mutations, to all types of inherited
afflictions, is beyond the scope of this book.) It seems to us
that anyone who contemplates Part 9 of this
chapter, on known
methods of dose-reduction in radiology, has to ask: Why wait?
What is the purpose of waiting, when only benefit, and no harm,
can come from reducing uselessly high doses as rapidly as
possible?
10e. A
Mountain of Solid Evidence That Each Dose Matters
The
fact, that xray doses are so seldom measured, reflects the
false assumption that such doses do not matter. This monograph
has presented a mountain of solid evidence that they do matter,
enormously. And each bit of additional dose matters, because
any xray photon may be the one which sets in motion the
high-speed high-energy electron which causes a carcinogenic or
atherogenic mutation. Such mutations rarely disappear. The
higher their accumulated number in a population, the higher will
be the population's mortality-rates from radiation-induced
Cancer and Ischemic Heart Disease.
The
xray is a proven mutagen and a proven cause of Cancer, and
the evidence in this book strongly indicates that it is also a
very important cause of Cancer and a very important atherogen.
From the existing evidence, it is clear that average per patient
doses from diagnostic and interventional radiology could be
reduced by a great deal without reducing the medical benefits of
the procedures in any way (Part 9, above): Same procedures, at
lower doses. Unless effective measures are taken, to eliminate
uselessly high dosage, medical radiation will continue in the
next century to be a leading cause of Cancer and Ischemic Heart
Disease in the United States, and will become a leading cause in
the "developing" world, too.
10f. A
Prudent Position from Which No One Loses, Everyone Gains
Whether
diseases are common or rare, a prime reason for studying
their causation is prevention. Cancer and Ischemic Heart
Disease, combined, accounted for 45% of all deaths in the USA
during 1993 (Chapter 39, Part 4).
If
we in the medical professions take the position, that we
should not press for reducing doses from medical radiation until
every question has been perfectly answered, then we can never
un-do the harm inflicted during the waiting period, upon tens of
millions of patients every year. By contrast, if we take the
prudent position that dose-reduction should become a high
priority without delay (and if humans do not start exposing
themselves to some other potent mutagen), the evidence in this
monograph indicates that we will prevent much of the future
mortality from Cancer and Ischemic Heart Disease, without
causing any adverse effects on health. No one loses, everyone
gains.
>>>>>>>>>>
![]() Part
2. Some Key Facts about Xrays and Ionizing Radiation in General
Part
2. Some Key Facts about Xrays and Ionizing Radiation in General
![]() Part
3. No Doubt about Benefits from Medical Radiation
Part
3. No Doubt about Benefits from Medical Radiation
![]() Part
4. Role of Medical Radiation in Causing Cancer and IHD, Past and Present
Part
4. Role of Medical Radiation in Causing Cancer and IHD, Past and Present
![]() Hypothesis-1: Medical radiation is a highly important
cause (probably the principal cause) of cancer mortality in the
United States during the Twentieth Century. Medical radiation
means, primarily but not exclusively, exposure by xrays ---
including fluoroscopy and CT scans. (Hypothesis-1 is about
causation of Cancer, so it is silent about radiation-therapy
used after a Cancer has been diagnosed.)
Hypothesis-1: Medical radiation is a highly important
cause (probably the principal cause) of cancer mortality in the
United States during the Twentieth Century. Medical radiation
means, primarily but not exclusively, exposure by xrays ---
including fluoroscopy and CT scans. (Hypothesis-1 is about
causation of Cancer, so it is silent about radiation-therapy
used after a Cancer has been diagnosed.)
![]() Hypothesis-2: Medical radiation, received even at very
low and moderate doses, is an important cause of death from
Ischemic Heart Disease (IHD); the probable mechanism is
radiation-induced mutations in the coronary arteries, resulting
in dysfunctional clones (mini-tumors) of smooth muscle cells.
(The kinds of damage to the heart and its vessels, observed from
very high-dose radiation and reported for decades, seldom
resemble the lesions of IHD --- details in Appendix J.)
Hypothesis-2: Medical radiation, received even at very
low and moderate doses, is an important cause of death from
Ischemic Heart Disease (IHD); the probable mechanism is
radiation-induced mutations in the coronary arteries, resulting
in dysfunctional clones (mini-tumors) of smooth muscle cells.
(The kinds of damage to the heart and its vessels, observed from
very high-dose radiation and reported for decades, seldom
resemble the lesions of IHD --- details in Appendix J.)
 All-Cancers-Combined, m 1940 90% 1988 74%
All-Cancers-Combined, m 1940 90% 1988 74%
 All-Cancers-Combined, f 1940 58% 1988 50%
All-Cancers-Combined, f 1940 58% 1988 50%
 Breast Cancer, f 1940 ~ 100% 1990 83%
Breast Cancer, f 1940 ~ 100% 1990 83%
 All-Cancer-Except-Genital, f 1940 75% 1980 66%
All-Cancer-Except-Genital, f 1940 75% 1980 66%
 Ischemic Heart Disease, m 1950 79% 1993 63%
Ischemic Heart Disease, m 1950 79% 1993 63%
 Ischemic Heart Disease, f 1950 97% 1993 78%
Ischemic Heart Disease, f 1950 97% 1993 78%
![]() Part
5. Our Method for Calculating Fractional Causation
Part
5. Our Method for Calculating Fractional Causation
![]() An R-squared value of 1.00 is perfection. An R-squared value
of 0.70 is very good. Those who are familiar with the
correlation coefficient, R, will recognize that R-squared values
are lower than the corresponding R-values (for instance, when R
= 0.83666, R-squared = 0.70; when R = 0.94868, R-squared =
0.90).
An R-squared value of 1.00 is perfection. An R-squared value
of 0.70 is very good. Those who are familiar with the
correlation coefficient, R, will recognize that R-squared values
are lower than the corresponding R-values (for instance, when R
= 0.83666, R-squared = 0.70; when R = 0.94868, R-squared =
0.90).
![]() A ratio of (X-Coef/S.E.) of about 2.0 generally indicates a
statistically significant correlation. A ratio of 4.0 is a
tight correlation. A ratio above 4.0 is very tight. The ratio
describes the reliability of the slope in a line of best fit.
A ratio of (X-Coef/S.E.) of about 2.0 generally indicates a
statistically significant correlation. A ratio of 4.0 is a
tight correlation. A ratio above 4.0 is very tight. The ratio
describes the reliability of the slope in a line of best fit.