Part 1. The Estimate of 75 %
The number of radiation-induced breast-cancer cases per
year in the USA is estimated as 114,336 cases in
the Master Table
(sum of Column-W
entries), not rounded-off. This number is (114,336 /
182,000), or 63 percent of the annual total incidence,
if yearly production = yearly delivery.
What If the Dose Was Really Twice What Is Evaluated in the Master Table?
We believe that our Master Table seriously underestimates the annual average breast-dose in the 1920-1960 period. We believe that the true dose was probably at least twice the estimate in the Master Table from all sources combined, for the reasons discussed in Chapter 38 --- especially the omitted doses from fluoroscopy and from treatment of both skin and inflammatory conditions.
Despite its probably large underestimate, the Master Table indicates that past radiation is responsible for about 63 % of the recent, current, and future breast-cancer problem in the USA. If the annual average breast-dose, in person-rads, were really at least twice what we estimated, are we saying something absurd: That more than 100 % of the breast-cancer problem is radiation-induced?
Of course not. 100 % of a problem is "the max."
If the annual average dose was at least twice what was estimated in the Master Table, would it mean that the estimated conversion-factors need reduction? It might mean that. And it might not. It might mean that the number of new breast-cancer cases "delivered" per year is going to rise above 182,000, and that additional cases are going to be radiation-induced. Even the inherited "destiny" cases may require help from radiation and other non-inherited factors, as discussed in Chapter 1, Part 5.
This comment on the underestimation of dose, however, does not mean that we are "married" to any particular set of conversion-factors. No matter who proposes conversion-factors, such factors necessarily combine real-world evidence with some assumptions. If future evidence invalidates some of those assumptions, objective analysts will discard the assumptions without hesitation.
This study uses a current set of reasonable conversion-factors --- and they are appropriate for the initial inquiry. Still, we would like to point out (A) that these conversion-factors take no account of individuals who develop more than one radiation-induced breast-cancer, and (B) that the conversion-factors are lifetime factors which take no account of when breast cancer occurs --- even though it makes a big difference to breast-cancer patients whether it occurs at age 30 or at age 80. We regard this study as the beginning, not the end, of such inquiries.
Part 2. Some Intriguing Questions for Future Resolution
An underlying assumption in the Master Table is that conversion-factors remain valid in a population, decade after decade. That is a reasonable assumption if all other carcinogenic forces remain constant. With respect to breast-cancer, many of these other forces are not yet identified with certainty.
No matter how high is the percentage for breast-cancer's radiation etiology, it is important to learn how other agents and events (e.g., childbirth) also participate in breast-cancer development, as emphasized in Chapter 1, Part 5. For instance, interaction of other agents and events with ionizing radiation may make matters worse, by permitting radiation-induced breast-cancers to appear earlier than they otherwise would. Such information would be of great interest.
The world is a long way from knowing how to quantify the net interaction of ionizing radiation with other carcinogens. Indeed, we do not even know yet whether some of the non-radiation risk-factors for breast-cancer operate by inducing permanent genetic lesions, or by inappropriately turning critical genes off-or-on (without inflicting any permanent molecular injury), or by some other mechanism. We do not know whether the non-radiation risk-factors require the presence of permanent radiation-induced lesions in order to have their effect --- or vice versa, with radiation-induced lesions requiring the presence of non-radiation factors --- or whether all these factors are independent of each other. These are important and intriguing questions.
Disappearance of the Excess Relative Risk
Even if the factors act independently at the cellular level, there is the potential for severe confounding of studies by chronic exposure to a single agent, like ionizing radiation. For example, suppose (for the sake of simplification) that ionizing radiation is the only cause of breast-cancer. And suppose that we do a study in which we carefully observe the A-bomb survivors (or female nuclear workers, etc.) to compute the percent increase in the apparent "spontaneous rate" of breast-cancer per rad over full lifespans.
If we fail to take into account that the apparent "spontaneous" rate is rising equally both in the comparison-groups and in the matched control-groups, due to equal amounts of medical irradiation, we are going to underestimate the Excess Relative Risk per rad (Chapter 3, Part 3). In fact, one implication of the "Law of Equality" is that exposure of a stable population to a constant level of ionizing radiation would --- at equilibrium --- cause no increase per rad in the apparent "spontaneous" rate, even if radiation were causing 100 % of the problem.
Another Potential Pitfall in Studies of Cancer-Causation
It is well worth noting that, among risk-factors for breast-cancer, not all have been studied with respect to the full lifespan of women. We do not doubt the validity of observations which correlate the presence of various non-radiation risk-factors with elevated rates of breast-cancer, and conversely, correlate their absence with reduced rates of breast-cancer. But we regard the "lift-off" phenomenon described in Chapter 3 (Part 4) as a potential pitfall in non-lifespan studies.
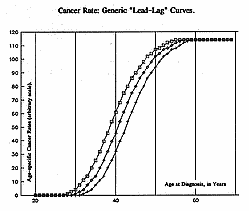 The figure at right depicts three curves under which the lifetime
area is not very different. Suppose the middle curve
depicts the age-specific breast-cancer rate, for which we use
an arbitrary scale. Suppose (for simplification)
that the middle curve is due exclusively to
ionizing radiation.
The figure at right depicts three curves under which the lifetime
area is not very different. Suppose the middle curve
depicts the age-specific breast-cancer rate, for which we use
an arbitrary scale. Suppose (for simplification)
that the middle curve is due exclusively to
ionizing radiation.
Next, let us suppose that presence of some additional factor shifts the middle curve just slightly to the left (to earlier ages, so we can call it the "lead" curve). Investigators will observe some big differences in rates as the two curves "lift-off" at slightly different ages from the baseline of zero. It is easy to observe 10-fold, 4-fold, and 100 % increases over several years of study. Nonetheless, the factor causing the big increases does not have much more area under its lifetime "lead" curve than the area under the middle curve, due to radiation alone. In this illustration, a failure to have lifetime data on the non-radiation factor could result in erroneous assumptions about its real, lifetime impact.
Lastly, let us suppose that presence of some additional factor shifts the middle curve just slightly to the right (to older ages, so we can call it the "lag" curve). Investigators will observe some big differences in rates as the two curves "lift-off" at slightly different ages from the baseline of zero. Nonetheless, the factor causing the big "protection" does not have much less area under its lifetime "lag" curve than the area under the middle curve, due to radiation alone. In this illustration, a failure to have lifetime data on the non-radiation factor could lead to erroneous assumptions about its real, lifetime impact.
For ionizing radiation, the Atomic Bomb Study evaluates the lifetime carcinogenic effect of exposure upon its participants, with completion approaching even for the youngest ages at exposure. We can not overemphasize the unique value of the A-Bomb Study, and the importance of maintaining a single continuous set of cohorts until the study is complete.
Importance of Exact Age-Matching in Epidemiologic Cancer-Studies
The "Lead-Lag" Curves illustrate another potential pitfall in epidemiologic cancer-studies. Suppose we are doing a prospective study to learn if an X-type-diet (or pharmaceutical, or whatever) has any effect on the rate of breast-cancer. And suppose that the experimental group on an X-type-diet and the control group are quite well matched --- except that the Diet-X group is older by just a few years. All three curves in the figure reflect the fact that, after "lift-off," a few additional years mean an appreciable increase in cancer-rate, when the curves are steep. A difference of two years in age can mean a difference in rates which is not negligible.
So the figure illustrates why epidemiologic studies simply can not ignore small differences in age. In the Diet-X Study, if we observe a higher rate of breast-cancer in the Diet-X women, we had better pay close attention to the small difference in age. It might explain everything.
Part 3. The Key Certainties about Our Finding
In this chapter and in earlier ones, we have pointed to various approximations and uncertainties in our study. Now, it is time to summarize some of the underlying certainties.
We stated at the outset (Chapter 1) that causation of extra breast-cancer by ionizing radiation is proven --- it is not a speculation. And in this book's Reference list, we flag (with # ) some of the papers which present the evidence of causation and quantify the risk from various studies. With respect to irradiated groups, "risk" does not mean "maybe" --- it means the observed rate of radiation-induced breast-cancer.
This is another observation which is not in doubt (Chapter 2). In order to evaluate the contribution of radiation to recent, current, and future breast-cancer incidence, we must include radiation exposures which occurred decades earlier.
The evidence for this is clear, now (Chapter 3). The increase shows up first in extra cases of early-onset breast-cancer, and the increased rate continues for at least 40 years after the exposure.
Comparisons between different ages at irradiation are made meaningful on the basis of the lifetime response. The comparisons necessarily incorporate approximations for the younger age-groups, because their lifetime follow-up is not yet complete in the A-Bomb Study. Over the past twenty years, comparisons have become increasingly reliable, as observations of the younger groups gradually replace approximations.
Is it reasonable to regard the elevated sensitivity of the young as a certainty?
In the Tokunaga Study --- specifically of breast-cancer incidence in the A-Bomb Study for 1950-1985 --- the analysts have presented Excess Relative Risks per sievert for six age-groups (age at the time of the bombings). At 40 years post-bombing, they report that the Excess Relative Risk is 10-fold higher for age-years 0-9 than for age-years 50+ (Tokunaga 1994, Table 6, p.215).
What is the estimated lifetime ratio in our independent conversion-factors? It is (92.74 / 24.56), or only 3.78. The ratio would have been 7.55-fold if we had not slashed the conversion-factor in half for the 0-9 year-olds (see Chapter 40, Box 6, Column R). We made this downward adjustment because we know that the interim observations are affected by the "lift-off" factor. Therefore, the interim observations must decline somewhat by the end of the lifetime follow-up.
With the difference in age-sensitivity still as large as 10-fold or 7.5-fold, it is extremely unlikely that the sensitivity will completely disappear. We can classify the special sensitivity of the young as a certainty, with respect to radiation-induced breast-cancer.
This observation is discussed in Chapter 40, in the text for Box 6. The observation comes from the 1994 Thompson Study of cancer incidence (all sites) in the A-Bomb Study, 1958-1987. Breast-cancer shows by far the highest Excess Relative Risk per sievert in the study. By comparison with all cancer-sites combined, breast-cancer is 2.524-fold more inducible per unit of radiation.
This observation was mentioned in Chapter 5, Part 5, and will be further discussed in Chapter 42.
We recommend that readers keep this short list of certainties in their minds. The list will keep some responses to this book in perspective.