Published by:
Committee for Nuclear Responsibility. Tel 415-776-8299.
Hardcover: ISBN 0-932682-97-9. $35.00. Paperback: ISBN 0-932682-98-7. $27.00.
Paper in both editions is pH neutral. There are 699 pages per book,
and page-size is 8.5 x 11 inches upright (21.6 x 27.9 cm).
Both the hardcover and softcover editions are sturdy and durable.
The hardcover has a glossy laminated casing (no jacket); the
textblock is Smyth-sewn. Librarians can obtain additional details
about the binding from the publisher.
- What We Do Know about Heart Attacks. 1957.
- Dietary Prevention and Treatment of Heart Disease.
Co-authors: Alex V. Nichols and E. Virginia Dobbin. 1958. LCCN 58-10072.
- Coronary Heart Disease. 1959. LCCN 58-14073.
- Radiation and Human Health. 1981. LCCN 80-26484.
- Xrays: Health Effects of Common Exams.
Co-author: Egan O'Connor. 1985. LCCN 84-23527.
- Radiation-Induced Cancer from Low-Dose Exposure: An Independent
Analysis. 1990. LCCN 89-62431.
- Chernobyl Accident: Radiation Consequences for This and Future
Generations. 1994. ISBN 5-339-00869-X
(Vysheishaya Shkola Publishing House, Minsk, Belarus).
- Preventing Breast Cancer: The Story of a Major, Proven,
Preventable Cause of This Disease. 1995/96.
LCCN 94-69129 (lst edition, 1995). LCCN 96-2453 (2nd edition, 1996).
The publisher takes great pleasure in thanking the following individuals and foundations for their support of CNR's publishing program on the health effects of exposure to ionizing radiation:
June Allen, M.Ed.
Phillip M. Allen, M.D., Ph.D.
Rodney Baird, in memoriam
Charles Bloomstein
David C. Bradley, M.D.
Paul F. Burmeister
Columbia Foundation
C.S. Fund
Richard Dorwin Davis, in memoriam
Leo and Kay Drey
Genevieve Ellis Estes, in memoriam
Robin M. Fleck, M.D.
Friendship Fund
Franklin L. Gage
John B. Gilpin
Richard and Rhoda Goldman Fund
The Grodzins Fund
Anne D. Hahn, in memoriam
Hahn Family Foundation
Betty Rhodes Latner
Robert Lowitz
James P. McGinley, M.D.
Mary R. Morgan
David T. Ratcliffe
Right Livelihood Award Foundation
Caroline H. Robinson Social Service Fund
Lawrence G. Tesler
May C. Tooker
SECTION ONE
Orientation, Materials, Methods
Introduction ........................................................................... 1
Abstract ............................................................................... 5
Chap.1 Executive Summary of This Book ......................................................... 7
2 Pre-1960 and Post-1960 Uses of Medical Radiation, and Its Carcinogenic Action .......... 27
3 PhysPops --- The Doses in Some Massive Studies of Dose-Response ........................ 53
4 Mortality Rates --- The Responses in the Dose-Response Studies ......................... 77
5 Dose-Response, Linear Regression, and Some Other Key Concepts in Our Analyses .......... 89
SECTION TWO
Cancer Mortality: Evidence that Medical Radiation Became a Principal Cause by 1940
6 All-Cancers-Combined, Males: Relation with Medical Radiation .......................... 107
7 All-Cancers-Combined, Females: Relation with Medical Radiation ........................ 119
8 Breast Cancer, Females ................................................................. 125
9 Digestive-System Cancers, Males ........................................................ 131
10 Digestive-System Cancers, Females ...................................................... 137
11 Urinary-System Cancers, Males .......................................................... 143
12 Urinary-System Cancers, Females ........................................................ 149
13 Genital Cancers, Males ................................................................. 155
14 Genital Cancers, Females ............................................................... 161
15 Buccal-Cavity & Pharynx Cancers, Males ................................................. 169
16 Respiratory-System Cancers, Males ...................................................... 175
17 Respiratory-System Cancers, Females .................................................... 181
18 "Difference" Cancers (All-minus-Respiratory), Males .................................... 187
19 "Difference" Cancers (All-minus-Respiratory), Females .................................. 193
20 All-Cancer-Except-Genital-Cancer ....................................................... 199
21 All-Cancer Except (Genital + Respiratory) .............................................. 205
22 Summarized Results of Chapters 6 - 21, and Discussion .................................. 209
SECTION THREE
NonCancer NonIHD Mortality: Inverse Dose-Response with Medical Radiation
23 All Causes of Death Combined: Relation with Medical Radiation ......................... 223
24 All Causes of Death Except Cancer ...................................................... 229
25 All Causes of Death Except (Cancer + Ischemic Heart Disease) ........................... 233
26 Appendicitis, Deaths ................................................................... 238
27 CNS Vascular-Lesions (Strokes), Deaths ................................................. 241
28 Chronic Nephritis, Deaths .............................................................. 244
29 Diabetes Mellitus, Deaths .............................................................. 247
30 Hypertensive Disease, Deaths ........................................................... 250
31 Influenza and Pneumonia, Deaths ........................................................ 253
32 Fatal Motor-Vehicle Accidents .......................................................... 256
33 Other Fatal Accidents .................................................................. 259
34 Rheumatic Fever & Rheumatic Heart Disease .............................................. 262
35 Syphilis and Sequelae, Deaths .......................................................... 265
36 Tuberculosis, Deaths ................................................................... 267
37 Ulcer of Stomach and Duodenum, Deaths .................................................. 270
38 Summary on NonCancer NonIHD Results: Facts "Demanding" an Explanation ................. 272
SECTION FOUR
Ischemic Heart Disease: Evidence that Medical Radiation Became an Important Cause by 1950
39 Ischemic Heart Disease: Medical Radiation as a Cause ................................... 275
40 IHD in Males: The Dose-Response between Medical Radiation and IHD ...................... 279
41 IHD in Females: The Dose-Response between Medical Radiation and IHD .................... 289
42 Similarities in the IHD and Cancer Findings: Tumors in Both Diseases? .................. 295
43 Nature of Atherosclerotic Lesions Underlying IHD ........................................ 299
44 Some "Schools" of Thought on IHD Etiology and on IHD Acute Fatal Events ................. 305
45 Unified Model: Intersection of Lipoproteins & Dysfunctional Clones of SMCs ............. 337
46 How the Unified Model Helps to Explain, or Relates to, Other Observations ............... 345
SECTION FIVE
Cancer and IHD Mortality after 1940: Fractional Causation by Medical Radiation
47 Evaluating Fractional Causation in the Post-1940 Decades: How We Start ................. 355
48 Cigarette Smoking: When, Who, How Much, and Especially Where ........................... 361
49 All-Cancers, Males, 1940-1988: Fractional Causation by Medical Radiation ............... 375
50 All-Cancers, Females, 1940-1988: Fractional Causation by Medical Radiation ............. 387
51 Respiratory-System Cancers, Males, 1940-1988 ............................................ 393
52 Respiratory-System Cancers, Females, 1940-1988 .......................................... 405
53 Difference-Cancers, Males, 1940-1988 .................................................... 411
54 Difference-Cancers, Females, 1940-1988 .................................................. 417
55 Breast-Cancers, Females, 1940-1990 ...................................................... 423
56 All-Cancers-Except-Genital, Females, 1940-1980 .......................................... 429
57 Digestive-System Cancers, Males, 1940-1988 .............................................. 435
58 Digestive-System Cancers, Females, 1940-1988 ............................................ 441
59 Urinary-System Cancers, Males, 1940-1980 ................................................ 447
60 Urinary-System Cancers, Females, 1940-1980 .............................................. 455
61 Genital Cancers, Males, 1940-1990 ....................................................... 461
62 Genital Cancers, Females, 1940-1980 ..................................................... 467
63 Buccal-Pharynx Cancers, Males, 1940-1980 ................................................ 469
64 Ischemic Heart Disease, Males, 1950-1993 ................................................ 477
65 Ischemic Heart Disease, Females, 1950-1993 .............................................. 483
66 Summarized Results, from Evidence Which Spans about a Half-Century ...................... 489
SECTION SIX
The Status of Hypotheses One and Two
67 Our Findings: In Conflict with Existing Evidence? ...................................... 495
68 Is There a Reasonable Non-Radiation Explanation for the Observations? ................... 507
69 Conclusion: Making Sense of Three Sets of Irrefutable Correlations ..................... 513
APPENDICES
App A Dose-Units and Dose-Levels of Ionizing Radiation ........................................ 517
App B The Safe-Dose Fallacy: Summary of Three Remarkably Similar Reports ..................... 521
App C The Free-Radical Fallacy about Ionizing Radiation: A Demonstration ..................... 530
App D Radiation-Induced Genomic Instability: What It Is, and Why It Is Important ............. 533
App E Some Pathways toward Understanding the Atherogenic Role of Lipoproteins ................. 538
App F Dietary Advice in Prevention and Management of Ischemic Heart Disease ................... 555
App G Any Goodness in "Good Cholesterol" ? .................................................... 577
App H "Small, Dense Lipoprotein Particles" Especially Atherogenic?: Basis for Strong Doubt ... 586
App I "Snapshot" Epidemiology: Why Lipid Levels Seemed Less Important at Older Ages .......... 594
App J Coronary Effects of Very High-Dose Medical Radiation .................................... 599
App K Mid-Century: Average Annual Per Capita Dose from Diagnostic Medical Xrays .............. 609
App L Radiation "Hormesis": How an Illusion Can Arise from "Perfectly Good Data" ............. 617
App M Fractional Causation, 1980-1993, after an Alternate Smoking Adjustment .................. 621
App N PhysPop Omitted: Correlations between Canc. & IHD MortRates (Past, Present) ............ 642
Reference List .................................................................................. 645
Index and Glossary .............................................................................. 677

The Author's History
by Egan O'Connor
John William Gofman is Professor Emeritus of Molecular and Cell Biology, University of California at Berkeley, CA 94720-5706. He is also on the faculty at the University of California Medical School at San Francisco (UCSF). His life's work is divisible into three main areas, which converge for the first time in this monograph. Some of the earlier work is cited in the monograph's Reference List* (1) While a graduate student at U.C. Berkeley, Gofman earned his Ph.D. (1943) in nuclear/physical chemistry, with his dissertation on the discovery of Pa-232, U-232, Pa-233, and U-233, the proof that U-233 is fissionable by slow and fast neutrons, and discovery of the 4n + 1 radioactive series. His faculty advisor was Glenn T. Seaborg (who became Chairman of the Atomic Energy Commission, 1961-1971). Seaborg, Gofman, and Raymond W. Stoughton share Patent #3,123,535 on the slow and fast neutron fissionability of uranium-233, with its application to production of nuclear power or nuclear weapons. The work is recounted in Seaborg's book "Nuclear Milestones" (1972).
Post-doctorally, Gofman continued research related to the first atomic bombs --- particularly the chemistry of plutonium, at a time when the world's total supply was less than 0.25 milligram. He shares patents #2,671,251 and #2,912,302 on two processes for separating plutonium from the uranium and fission products of irradiated nuclear fuel. "We all were pushing the envelope in those years, and in the process, we learned the habit of observing details very closely."
* (2) After the plutonium work, Gofman completed medical school (1946) at UCSF, where the faculty and his classmates selected him to receive the annual Gold-Headed Cane Award for having the qualities of "a true physician."
In 1947, following his internship in Internal Medicine, Gofman joined the faculty at U.C. Berkeley (Division of Medical Physics), where he began his research on lipoproteins and Coronary Heart Disease at the Donner Laboratory. At the time, only two types of blood lipoproteins were known: Alpha and beta. By devising special flotation techniques with the ultracentrifuge, he and Frank T. Lindgren and co-workers at the Donner Lab began to reveal (1949-1950) the great diversity of very-low-density, intermediate-density, low-density, and high-density lipoproteins (VLDL, IDL, LDL, HDL) which truly exist in the bloodstream.
Their work on the chemistry of lipoproteins (e.g., the cholesterol-rich and triglyceride-rich varieties), and on dietary experiments, and on epidemiologic studies, soon produced evidence that high blood levels of the LDL, IDL, and VLDL lipoproteins are a risk-factor for Coronary Heart Disease.
In 1954, Gofman received the Modern Medicine Award for outstanding contributions to heart disease research. In 1965, he received the Lyman Duff Lectureship Award of the American Heart Association, for his research in atherosclerosis and Coronary Heart Disease. In 1972, he shared the Stouffer Prize for outstanding contributions to research in arteriosclerosis. In 1974, the American College of Cardiology selected him as one of twenty-five leading researchers in cardiology of the past quarter-century.
* (3) Meanwhile, in the early 1960s, the Atomic Energy Commission (AEC) asked Gofman to establish a Biomedical Research Division at the AEC's Livermore National Laboratory, for the purpose of evaluating the health effects of all types of nuclear activities. From 1963-1965, Gofman served as the division's first director and concurrently as an Associate Director of the full laboratory. Then he stepped down from the administrative activities in order to have more time for his own laboratory research on Cancer and chromosomes (the Boveri Hypothesis), on radiation-induced chromosomal mutations and genomic instability, and for his analytical work on the epidemiologic data from the Japanese atomic-bomb survivors and other irradiated human populations.
By 1969, Gofman and a Livermore colleague, Dr. Arthur R. Tamplin, had concluded that human exposure to ionizing radiation was much more serious than previously recognized. Because of this finding, Gofman and Tamplin spoke out publicly against two AEC programs which they had previously accepted. One was Project Plowshare, a program to explode hundreds or thousands of underground nuclear bombs in the Rocky Mountains in order to liberate (radioactive) natural gas, and to use nuclear explosives also to excavate harbors and canals. The second was the plan to license about 1,000 commercial nuclear power plants (USA) as quickly as possible. In 1970, Gofman and Tamplin proposed a 5-year moratorium on that activity.
The AEC was not pleased. Seaborg recounts some of the heated conversations among the Commissioners in his book The Atomic Energy Commission under Nixon: Adjusting to Troubled Times (1993). By 1973, Livermore de-funded Gofman's laboratory research on chromosomes and Cancer. He returned to teaching full-time at U.C. Berkeley, until choosing an early and active "retirement" in order to concentrate fully on pro-bono research into human health-effects from radiation.
His 1981, 1985, 1990, 1994, and 1995/96 books present a series of findings. His 1990 book includes his proof, "by any reasonable standard of biomedical proof," that there is no threshold level (no harmless dose) of ionizing radiation with respect to radiation mutagenesis and carcinogenesis --- a conclusion supported in 1995 by a government-funded radiation committee. His 1995/96 book provides evidence that medical radiation is a necessary co-actor in about 75% of the recent and current Breast Cancer incidence (USA) --- a conclusion doubted but not at all refuted by several peer-reviewers.
John W. Gofman is the son of David and Sarah Gofman --- who immigrated to the USA from czarist Russia in about 1905. JWG was born in Cleveland, Ohio, in September 1918.
INTRODUCTION
Overview, and Some Practical Implications of This Work
Part 1. Practical Implications of Hypotheses One and Two
Part 2. Differing Origins of the Two Hypotheses
Part 3. Some Rather Dazzling Results to Examine
Part 4. Why Our Findings Do Not Challenge the Importance
of Other Causes of Cancer and IHD
Part 5. How to Reconcile High Fractional Causations by Xrays, Smoking, Diet
* Part 1. Practical Implications of Hypotheses One and Two
During the 1990s, approximately 23% of the U.S. deaths have been caused by Cancer, and 22% by Ischemic Heart Disease (also called Coronary Heart Disease, and Coronary Artery Disease).
Would anyone not welcome a simple, safe, and painless way either to postpone many cases of such diseases or to prevent many cases from occurring at all? The findings in this book, combined with already-published wisdom from some mainstream radiologists and radiologic physicists, identify such a way --- with certainty for Cancer, and with great likelihood for Ischemic Heart Disease (IHD).
The word "practical" is featured above, because prevention of these two diseases has always been our chief reason for investigating their causes. The evidence assembled and analyzed in this monograph identifies medical radiation as a very important cause of both diseases. The work is organized around two hypotheses.
1a. Statement of Hypothesis-1 (Cancer) and Hypothesis-2 (IHD)
* Hypothesis-1 is this: Medical radiation is a highly important cause (probably the principal cause) of cancer mortality in the United States during the Twentieth Century. (Hypothesis-1 is about causation, so it is silent about radiation-therapy used after a Cancer has been diagnosed.)
We are well aware of a belief that medical radiation causes only a very low percentage of cancer mortality. That belief rests on a few estimates whose input-data are highly unreliable and sometimes inherently irrelevant, for the reasons presented in Chapters 1, 2, and 67 (Part 5). By contrast, the evidence in this book strongly supports Hypothesis-1. We are confident --- for the reasons listed in Chapter 1 --- that our findings are far more credible, scientifically, than the low estimates. Also we are confident, for reasons stated in Part 5, that our findings do not conflict with estimates that more than half of the cancer rate is a result of smoking and poor diet.
* Hypothesis-2 is this: Medical radiation, received even at very low and moderate doses, is an important cause of Ischemic Heart Disease (IHD); the probable mechanism is radiation-induction of mutations in the coronary arteries, resulting in dysfunctional clones (mini-tumors) of smooth muscle cells. (Here at the outset, we can prevent some confusion about Hypothesis-2 by stating that (a) it was discovered decades ago that medical radiation at very high doses can damage the heart and its vessels, and that (b) the kinds of damage reported from very high-dose radiation seldom resemble the lesions of Ischemic Heart Disease --- details in Appendix J.)
Chapter 45 presents a Unified Model of Atherogenesis and Acute IHD Events which is consistent with the evidence in this book, is consistent with the findings (first by Earl Benditt in 1973) of monoclonal cells in atherosclerotic plaques, is consistent with well-established knowledge about atherogenic lipoproteins and other non-xray causes of fatal IHD, and is consistent with recent findings about the weaker connection than expected between degree of arterial stenosis and the fatal rupturing of specific atherosclerotic plaques.
1b. What
Constitutes "Medical Radiation"?
Because not all readers will "arrive" here from the same fields, or with the same backgrounds, or with English as the native language, this book defines various terms and concepts in the fields of radiation, Cancer, Ischemic Heart Disease, and dose-response analysis. Definitions can be located with the combined Index and Glossary.
By medical radiation, Hypotheses One and Two mean primarily but not exclusively xrays (including fluoroscopy and CT scans).
There is no doubt that medical radiation can both be a cause of Cancer and also be used to treat Cancer. Cancerous activities are done by living cells, whose cancerous behavior can result from radiation-induced mutations of numerous types --- types which do not kill or sterilize the cells. When radiation is used for treatment of Cancer, it is used in very high doses which do enough damage to kill or sterilize cells. Clearly, dead or non-dividing cells cannot behave like cancer cells.
1c. Practical
Implications of Hypotheses One and Two
The validity of Hypotheses One and Two is a question with major implications for future health, in the USA and elsewhere. Validity means that medical professionals and other humans have, already at hand, an opportunity which is guaranteed to achieve large reductions in future mortality-rates from Cancer and which is very likely to achieve similar reductions in Ischemic Heart Disease, in countries where medical radiation is widely in use.
Knowledgeable "mainstream" experts in radiology and radiologic physics have shown that xray dosage, from nontherapeutic diagnostic and interventional radiology in current medicine, could readily be cut by a factor of two or more (Chapter 1, Box 3) --- while still obtaining all the benefits of such radiology and without eliminating a single procedure (specifics in Chapters 1 and 2). Example: While radiographers have reduced the xray dose per mammographic examination by more than 10-fold, use of mammography has risen dramatically. The result of dose-reduction has certainly not been less mammography --- but rather, less-risky mammography.
Beyond
diagnostic radiology, there is extensive and growing use
of xray fluoroscopy, nondiagnostically, during placement of
catheters and during surgical procedures. There is no doubt
that dosage could be reduced many-fold during such procedures
(Chapter 1, Box 3;
Chapter 2, Part 3).
How we happened to arrive at Hypothesis-1 is related in Chapter 2, Part 9. It deserves emphasis that Hypothesis-1 is not "Medical radiation can induce Cancer." Induction of Cancer in humans by ionizing radiation, including xrays, was proven long ago (Chapter 2, Part 4). The proof is so solid that it is accepted even by industries and professions which irradiate people.
Hypothesis-1 is that medical radiation causes a very large part of the nation's cancer problem. This book was undertaken in order to test, modify, or discard Hypothesis-1. In the process, the work also provides a bonus: Some of the most powerful evidence ever assembled confirming that ionizing radiation is a potent cause of virtually all types of human cancer.
By
contrast, ionizing radiation was not a proven cause of
Ischemic Heart Disease when Hypothesis-2 came into existence.
Hypothesis-2 "fell out of the data" which we assembled in order
to test Hypothesis-1. This book presents the first powerful
evidence that ionizing radiation is a cause of Ischemic Heart
Disease --- a very important cause.
In approximately 50 years of biomedical research, we have rarely seen support for an hypothesis (Hypothesis-1), and indication for a new hypothesis (Hypothesis-2), "fall out of data" so strongly as they do in this monograph. Such events have to be taken seriously by objective analysts.
Even
though the evidence is uncomplicated and the logic is
straightforward, this book is long because we have the unusual
policy of showing the steps which connect the raw data with the
conclusions. For readers who want to know only the "bottom
line," we provide an Abstract and Executive
Summary (Chapter 1).
of
Other Causes of Cancer and IHD
Both Cancer and Ischemic Heart Disease are well established as multi-cause diseases. There is convincing evidence that several different causes increase the death-rate from Cancer, and likewise, that several different causes increase the death-rate from IHD. Moreover, it is safe to say that multiple causes generally (perhaps always) contribute to a single case of fatal IHD, and to a single case of fatal Cancer. The case would not occur when it does, without co-action by multiple causes.
The concept of necessary co-actors is an old one. For instance, in the famous 1964 "Surgeon General's Report" on cigarette smoking as a cause of Lung Cancer, the authors wrote (p.31): "It is recognized that often the co-existence of several factors is required for the occurrence of a disease, and that one of the factors may play a dominant role; that is, without it, the other factors (such as genetic susceptibility) seldom lead to the occurrence of the disease."
The assumption, of more than one cause per case of Cancer, arises from various lines of evidence. For example, the rate of Breast Cancer is higher in women who inherit one mutated copy of a "Breast Cancer Gene" than in women without that inheritance, but that inheritance certainly does not guarantee the development of Breast Cancer in every breast-cell --- even though every breast-cell contains the mutation. One or more additional causes are necessary in order to turn even one of those breast-cells into a Cancer.
The concept, that more than one cause is necessary to produce a case of Cancer, is embraced by the widely accepted initiator-promoter model of Cancer. In that model, inherited or acquired carcinogenic mutations require help from a "promoter" --- for example, a hormone or infectious agent. The concept of mutually dependent co-actors is also inherent in the widely accepted multi-mutation multi-step models of carcinogenesis --- i.e., Cancer "is typically a multi-step process resulting from an accumulation of as many as 10 genetic changes in a single cell" (p.471 in Understanding Genetics: A Molecular Approach, Norman V. Rothwell; Wiley-Liss Publishers, 1993).
By definition, absence of a necessary co-actor prevents the result. When two or more co-actors each have a required role, in producing a particular case of disease, then the absence of any one of them will prevent the case. We would regard such co-actors as equally important.
Thus,
neither Hypothesis-1 nor Hypothesis-2 challenges the very
important roles, already established, for various nonradiation
causes of Cancer and IHD. When we propose that medical
radiation is a highly important cause of Cancer and IHD
mortality, we mean that in the absence of medical radiation,
many or most of the cases would not have occurred when they
did. While medical radiation has not been the only factor
contributing to such cases, we mean that it has been a necessary
co-actor in such cases. Discussion of co-action continues in
Chapter 6, Part 6.
Fractional Causation refers to the fraction of the cancer mortality rate which would be absent (prevented) in the absence of a specified carcinogen --- which is medical radiation, in this monograph. Therefore, Fractional Causation is the fraction or percentage of the cancer mortality rate attributable to medical radiation --- or caused by medical radiation, in ordinary parlance.
A related term, widely in use, is "radiation-induced Cancer." The term is a brief and convenient way to refer to cancer cases which would have been absent in the absence of exposure to ionizing radiation. It does not mean that radiation is necessarily the only cause contributing to cases of radiation-induced Cancer. Similarly, when people refer to "occupationally-induced Cancer," they do not mean that occupation is the only cause contributing to such cases. They refer to cases which would have been absent in the absence of occupational exposure to carcinogens.
An Illustration of 100 Cancer Cases Resulting from Co-Action
Suppose that the evidence in this book indicates that Fractional Causation by medical radiation, of the national cancer death-rate, is 90% in a certain decade. Because of co-action, such a finding would not leave only 10% for all other causes combined --- as we will illustrate here with some hypothetical values. We will limit our illustration to only four carcinogens: Xrays, smoking, poor diet, and particular inherited mutations. For brevity, we exclude other workplace, at-home, and environmental carcinogens. Then, we arbitrarily specify that the total cancer death-rate per year is 100 cases per 100,000 population and that these 100 cases are the result of co-action as follows. Our First List (illustrative):
- 40 cases by co-action of xrays + smoking + poor diet.
- 25 cases by co-action of xrays + poor diet + inherited mutations.
- 25 cases by co-action of xrays + smoking + inherited mutations.
- 10 cases by co-action of smoking + poor diet + inherited mutations.
The meaning of the first row, above, is that xrays, smoking, and poor diet each make a necessary contribution to each case of Cancer in the first row. In the absence of any one of the necessary co-actors, the 40 cases in the first row could not occur. That is the meaning of "necessary." The meaning is similar for all four rows of hypothetical values.
A Second List, also adding up to 100 cases, would have very different implications if it were: 90 cases caused by xrays acting alone, 4 cases caused by a dietary factor acting alone, 3 cases caused by smoking acting alone, and 3 cases caused by an inherited mutation acting alone. In both lists, the sum of cases = 100 cases, but every case in the First List is the result of more than one cause per case, whereas every case in the Second List is the result of only one cause per case (no co-action in the Second List).
The Illustrative Fractional Causations
by Xrays, Diet, Smoking, and Inherited Mutations
Out of the mixture of cases in the First List, we will explore how many cases could be prevented if we could remove just one cause, while the other causes remain as they were. Xrays are a required co-actor in (40 + 25 + 25), or 90 cases per 100 total cases. Because absence of a required co-actor prevents the result, 90% of the cancer death-rate would be absent, in the absence of exposure to medical radiation. Fractional Causation = 90% by medical radiation.
Next, we put radiation back into the mixture, and we remove just "poor diet." In our supposition, it is a required co-actor in (40 + 25 + 10), or 75 cases per 100 total cases. Because absence of a required co-actor prevents the result, 75% of the cancer death-rate would be absent, in the absence of poor diet in this illustration. Fractional Causation = 75% by poor diet. In our hypothetical illustration, Fractional Causation = 75% by smoking and 60% by inherited mutations. It is obvious that a high Fractional Causation by xrays does not require a low Fractional Causation by any other cause of Cancer.
Because Fractional Causation means the fraction or percentage of the death-rate which would be absent (prevented) by the absence of a specified co-actor, addition of the separate Fractional Causations produces nonsense (a total greater than 100%). Such addition would be equivalent to counting the same cases of absent Cancer more than once.
Our warning against adding Fractional Causations applies to a statement in the 1999 report of the National Research Council's sixth Committee on the Biological Effects of Ionizing Radiation (the BEIR-6 Report, from the National Academy Press, 1999). The BEIR-6 Committee, referring to evidence of co-action between smoking and exposure to radon (and radon's decay-products), states that "Some lung-cancer cases reflect the joint effect of the two agents and are in principle preventable by removing either agent" (BEIR-6, p.33). Although Fractional Causation of such cases is 100% by radon and 100% by smoking, addition of the two Fractional Causations would clearly count each prevented case twice.
Implications of Co-Action for Progress in Preventing Cancer and IHD
When more than one cause is required per case of Cancer or Ischemic Heart Disease, it means that reducing exposure to a single necessary carcinogen or atherogen reduces the impact of all its partners. If one can identify a single agent which is a necessary co-actor in a high fraction of cases of Cancer and Ischemic Heart Disease, one can make real progress in preventing these diseases by reducing exposure to that cause. The evidence uncovered in this book strongly indicates that medical radiation is such an agent.
ABSTRACT
Ischemic Heart Disease:
Dose-Response Studies with Physicians per 100,000 Population.
-
John W. Gofman, M.D., Ph.D. 1999. 699 pages. LCCN 99-045096.
Hardcover: ISBN 0-932682-97-9. Softcover: ISBN 0-932682-98-7.
Committee for Nuclear Responsibility Books, San Francisco.
ORIENTATION:
For decades, xrays and other classes of ionizing radiation have been a proven cause, in vivo and/or in vitro, of virtually all types of mutation --- especially structural chromosomal mutations (such as deletions, translocations, and rings), for which the doubling-dose by xrays is extremely low. Additionally, xrays are an established cause of in vitro genomic instability.
This monograph looks at the impact of medical radiation --- primarily from xrays, including fluoroscopy and CT scans --- upon mortality-rates from both Cancer and Ischemic (Coronary) Heart Disease, from mid-century to 1990. The evidence in this book strongly indicates that medical radiation has become a necessary co-actor (but not the only necessary co-actor) in causing over 50% of the death-rates from Cancer and Ischemic Heart Disease (IHD) --- a finding which is consistent with participation of non-xray causes as necessary co-actors in the same cases (Introduction). In multi-cause diseases such as Cancer and IHD, more than one necessary co-actor per fatal case is very likely. Absence of any necessary co-actor, by definition, prevents such cases. The concept, of cases due to medical radiation, means cases which would be absent in the absence of medical radiation.
PURPOSE:
Xrays have been a well-established cause of human Cancer for decades. This monograph was undertaken (a) to quantify what share of U.S. age-adjusted cancer mortality, for each gender, is caused by medical radiation, and (b) to check on the author's 1995 finding, based on completely different data, that exposure to medical radiation accounts for about 75% of Breast Cancer incidence in the USA. In the process of evaluating cancer mortality vs. noncancer mortality for this monograph, it became obvious that the impact of medical radiation upon death-rates specifically from Ischemic Heart Disease also demanded evaluation.
MATERIALS AND METHODS:
This study is based on mortality rates among 130-250 million persons --- namely, the entire United States population, 1940-1990. Age-adjusted cancer mortality rates (MortRates) per 100,000 population are available by gender for each of the Nine Census Divisions (USA), for the 1940-1990 decades, from Vital Statistics. Such rates for noncancer mortality rates also are available. For Ischemic Heart Disease, such rates are available starting in 1950, which means that NonCancer NonIHD MortRates, by Census Divisions, are available starting in 1950.
For reasons presented in Chapter 2 (Parts 2+3), there are no reliable estimates of average per capita population dose, accumulated from medical radiation, currently or in the past. Also not available, for reasons presented in Chapter 2 (Part 7c), are reliable estimates of cancer-risk per unit of dose from medical xrays. This monograph avoids these two types of uncertainty by using the number of physicians per 100,000 population (PhysPop) as a reasonable approximation of the relative magnitude of exposure from medical radiation in the Nine Census Divisions. The ranking of averaged PhysPop values by Census Divisions, over the 1940-1990 period, is remarkably stable.
MortRates are regressed upon PhysPop values, by Census Divisions, to determine the presence and direction of any dose-response. When a significant positive dose-response exists, the line of best fit is extended to the y-axis, where the intercept's value indicates what the MortRate would have been for that disease, if there had been no physicians per 100,000 population in a Census Division. The national MortRate for the disease under study, minus the intercept's value, provides a reasonable estimate of the share of that national MortRate which is due to medical radiation (i.e., the share which would be absent in the absence of medical radiation). Confidence limits are provided in Chapter 22, Box 1.
RESULTS:
Cancer and IHD MortRates each have very significant positive correlations with PhysPop, for males and females separately. By contrast, NonCancer NonIHD MortRates have a significant negative correlation with PhysPop. The following groups of Cancer were studied: All-Cancers-Combined, Breast Cancers, Digestive-System Cancers, Urinary-System Cancers, Genital Cancers, Buccal/Pharynx Cancers, Respiratory-System Cancers, Difference-Cancers (All-Except-Respiratory). Only female Genital Cancers failed to have a significant positive dose-response with PhysPop. The percentages, of the death-rates from Cancer and IHD caused by medical radiation (i.e., the shares which would be absent, in the absence of medical radiation), are shown in Box 1 of Chapter 1. For example:
Year Percent Year Percent
* All-Cancers-Combined, m 1940 90% 1988 74%
* All-Cancers-Combined, f 1940 58% 1988 50%
* All-Cancer-Except-Genital, f 1940 75% 1980 66%
* Breast Cancer, f 1940 ~ 100% 1990 83%
* Ischemic Heart Disease, m 1950 79% 1993 63%
* Ischemic Heart Disease, f 1950 97% 1993 78%
The growing impact of cigarette-smoking (Chapters 48, 49) almost certainly explains why the shares from medical radiation in 1980-1993 are somewhat lower than in 1940-50.
CONCLUSIONS:
Since its introduction in 1896, medical radiation has become a necessary co-actor in most fatal cases of Cancer and Ischemic Heart Disease (IHD).
It is proposed that, for radiation-induced IHD, the probable mechanism is radiation-induction of mutations in the coronary arteries, resulting in dysfunctional clones (mini-tumors) of smooth muscle cells. A Unified Model of Atherogenesis and Acute IHD Events is presented (Chapter 45), which is consistent with the findings in this book, is consistent with the findings (first by Earl Benditt in 1973) of monoclonal cells in atherosclerotic plaques, is consistent with well-established knowledge about atherogenic lipoproteins and other non-xray causes of fatal IHD, and is consistent with recent findings about the weaker connection than expected between degree of arterial stenosis and the fatal rupturing of specific atherosclerotic plaques.
The evidence in this monograph has major implications for prevention of Cancer and IHD. This monograph points to demonstrations, by others, of proven ways to reduce dose-levels of nontherapeutic medical radiation by 50% or considerably more, without eliminating a single diagnostic or interventional radiologic procedure and without degrading the information provided by medical radiation. Reduction of exposure to medical radiation can and will reduce mortality rates from both Cancer and Ischemic Heart Disease.
CHAPTER 1
Executive Summary of This Book
| Part 1. | Orientation: What Is Old, and What Is New |
| Part 2. | Some Key Facts about Xrays and Ionizing Radiation in General |
| Part 3. | No Doubt about Benefits from Medical Radiation |
| Part 4. | Role of Medical Radiation in Causing Cancer and IHD, Past and Present |
| Part 5. | Our Method for Calculating Fractional Causation |
| Part 6. | Eight Features Which Confer High Credibility on the Findings |
| Part 7. | Our Unified Model of Atherogenesis, and NonXray Co-Actors in IHD |
| Part 8. | A Personal Word: The Xray Deserves Its Honored Place in Health |
| Part 9. | Every Benefit of Medical Radiation: Same Procedures, Lower Dose-Levels |
| Part 10. | An Immense Opportunity: All Benefit, No Risk |
|
Boxes, Figures, and Tables, in that (alphabetical) order, are located in this book at the ends of the corresponding chapters. |
|
| Box 1. | Final Summary for Fractional Causation, by Medical Radiation, of Cancer and IHD. |
| Box 2. | Comparison of Dose-Response at Mid-Century: NonCancer NonIHD, Cancer, IHD. |
| Box 3. | Known Procedures Which Reduce Dosage from Medical Xrays. |
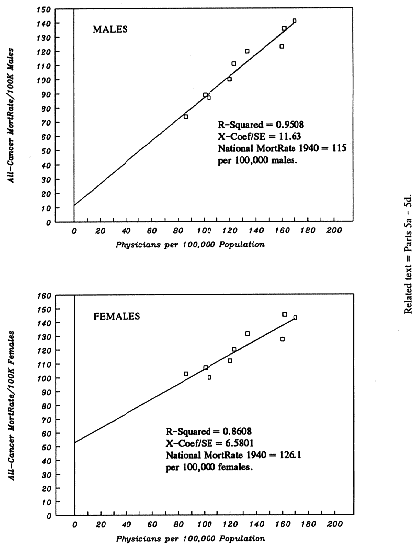
| Figure 1-A: | All-Cancers-Combined: Dose-Response between PhysPop and MortRates. |
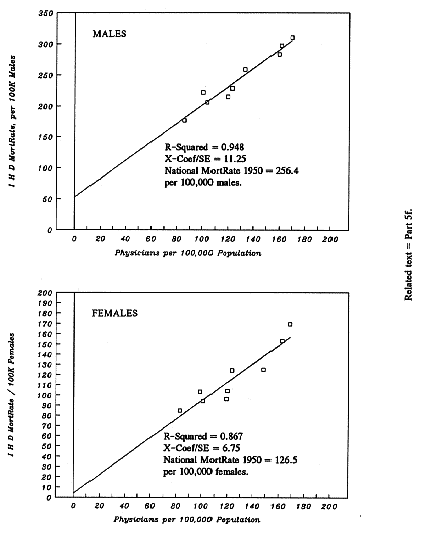
| Figure 1-B: | Ischemic Heart Disease: Dose-Response between PhysPop and MortRates. |
| Figure 1-C: | NonCancer NonIHD Deaths: Dose-Response between PhysPop and MortRates. |
* Part 1. Orientation: What Is Old, and What Is New
The evidence presented in this book strongly indicates that over 50% of the death-rate from Cancer today, and over 60% of the death-rate from Ischemic Heart Disease today, are xray-induced as defined and explained in Part 5 of the Introduction. The finding means that xrays (including fluoroscopy and CT scans) have become a necessary co-actor --- but not the only necessary co-actor --- in causing most of the death-rate from Cancer and from Ischemic Heart Disease (also called Coronary Heart Disease, and Coronary Artery Disease). In multi-cause diseases such as Cancer and Ischemic Heart Disease, more than one necessary co-actor per fatal case is very likely. Absence of any necessary co-actor, by definition, prevents such cases. The concept of xray-induced cases means cases which would be absent in the absence of exposure to xrays.
Xrays and other classes of ionizing radiation have been, for decades, a proven cause of virtually all types of mutations --- especially structural chromosomal mutations (such as deletions, translocations, and rings), for which the doubling dose by xrays is extremely low. Additionally, xrays are an established cause of genomic instability, often a characteristic of the most aggressive Cancers.
Not surprisingly, a host of epidemiologic studies have firmly established that xrays and other classes of ionizing radiation are a cause of most varieties of human Cancer. This monograph presents (a) the first compelling evidence that xrays are a cause also of Ischemic Heart Disease (IHD) --- a very important cause --- and presents (b) a Unified Model of Atherogenesis and Acute IHD Events (Part 7 of this chapter).
We have a high level of confidence that our findings, about the important causal role of medical radiation in both Cancer and IHD, are correct. Part 6 of this chapter identifies the features of the work which produce this confidence.
Part 9 of this chapter points to demonstrations, by others, of proven ways to reduce dose-levels of nontherapeutic medical radiation by 50% or considerably more, without eliminating a single diagnostic or interventional radiologic procedure and without degrading the information provided by medical radiation.
Reduction
of exposure to medical radiation can and will reduce
mortality rates --- from Cancer with certainty, and with very
great probability from Ischemic Heart Disease too.
Most physicians and other people appreciate the imaging capability of the xray, but --- through no fault of their own --- they are taught very little about the biological action of those xrays which never reach the film or other image-receptor. Part 2 provides some information about xrays and ionizing radiation in general. These facts are well supported in the peer-reviewed biomedical literature, in our text, and in our Reference List.
2a. Capacity
to Commit Mayhem among the Genetic Molecules
The biological damage from a medical xray procedure does not come directly from the xray photons. The damage comes from electrons, which those photons "kick" out of their normal atomic orbits within human tissues. Endowed with biologically unnatural energy by the photons, such electrons leave their atomic orbits and travel with high speed and high energy through their "home cells and neighboring cells. Each such electron gradually slows down, as it unloads portions of its biologically unnatural energy, at irregular intervals, onto various biological molecules along its primary track (path).
The molecular victims include, of course, chromosomal DNA, and the structural proteins of chromosomes, and water. Even though each energy-deposit transfers only a portion of the total energy of a high-speed high-energy electron, the single deposits very often have energies far exceeding any energy-transfer which occurs in a natural biochemical reaction. Such energy-deposits are more like grenades and small bombs (Chapter 2, Part 4a). None of this is in dispute.
2b. The
Free-Radical Fallacy
There is no doubt that, along the path of each high-speed high-energy electron described above, the energy-deposits produce various species of free radicals. Nonetheless, it is a demonstrated fallacy (Appendix-C) to assume equivalence between the biological potency of xrays and the biological potency of the free radicals which are routinely produced by a cell's own natural metabolism.
The uniquely violent and concentrated energy-transfers, resulting from xrays, are simply absent in a cell's natural biochemistry. As a result of these "grenades" and "small bombs," both strands of opposing DNA can experience a level of mayhem far exceeding the damage which metabolic free-radicals (and most other chemical species) generally inflict upon a comparable segment of the DNA double helix.
2c. Ionizing
Radiation: A Uniquely Potent Mutagen
The extra level of mayhem is what makes xrays (and other types of ionizing radiation) uniquely potent mutagens. Cells can not correctly repair every type of complex genetic damage, induced by ionizing radiation, and sometimes cells can not repair such damage at all (evidence discussed in Appendix-B and Appendix-C). Not all mutated cells die, of course. If they all died, there would be very little Cancer and no inherited afflictions. Indeed, certain mutations confer a proliferative advantage on the mutated cells. Exposure to xrays is a proven cause of genomic instability --- a characteristic of many of the most aggressive Cancers (Chapter 2, Part 4b, and Appendix-D).
Unlike some other mutagens, xrays have access to the genetic molecules of every internal organ, if the organ is within the xray beam. Within such organs, even a single high-speed high-energy electron, set into motion by an xray photon, has a chance (far from a certainty) of inducing the types of damage which defy repair. That is why there is no risk-free (no safe) dose-level (Appendix-B).
There is widespread agreement that, by its very nature, ionizing radiation at any dose-level can induce particularly complex injuries to the genetic molecules. There is growing mainstream acknowledgment that cellular repair processes are fallible, or entirely absent, for various complex injuries to the genetic molecules (Appendix-B and Appendix-C).
2d. The
Very Low Doubling-Dose for Xray-Induced Chromosomal
Mutations
The inability of human cells, to repair correctly every type of radiation-induced chromosomal damage, has been demonstrated in nuclear workers (who received their extra low-dose radiation at minimal dose-rates) and in numerous studies of xray-irradiated human cells at low doses. Besides demonstrating non-repair or imperfect repair, such studies have established that xrays have an extremely low doubling-dose for structural chromosomal mutations. (The doubling dose of an effect is the dose which adds a frequency equal to the pre-existing frequency of that effect.)
For instance, the doubling-dose for the dicentric mutation is in the dose range delivered by some common xray procedures, such as CT scans and fluoroscopy --- i.e., in the dose range of 2 to 20 rads (references in Chapter 2, Part 4b). The rad is a dose-unit which is identical to the centi-gray (Appendix-A). We, and many others, prefer the simpler name: Rad.
Xrays are capable of causing virtually every known kind of mutation --- from the very common types to the very complex types, from deletions of single nucleotides, to chromosomal deletions of every size and position, and chromosomal re-arrangements of every type. When such mutations are not cell-lethal, they endure and accumulate with each additional exposure to xrays or other ionizing radiation (Chapter 2, Part 8c; and Appendix-B, Part 2d).
2e. Medical
Xrays as a Proven Cause of Human Cancer
Ionizing
radiation is firmly established by epidemiologic
evidence as a proven cause of almost every major type of human
Cancer (Chapter 2,
Part 4c).
Some of the strongest evidence
comes from the study of medical patients exposed to xrays ---
even at minimal dose-levels per exposure (Appendix-B, Part 2d).
Mounting mainstream evidence indicates that medical xrays are 2
to 4 times more mutagenic than high-energy beta and gamma rays,
per rad of exposure (Chapter 2, Part 7).
Radiation was introduced into medicine almost immediately after discovery of the xray (by Wilhelm Roentgen) in 1895.
There is simply no doubt that the use of radiation in medicine has many benefits. The findings in this book provide no argument against medical radiation. The findings do provide a powerful argument for acquiring all the benefits of medical radiation with the use of much lower doses of radiation, in both diagnostic and interventional radiology. (Interventional radiology refers primarily, but not exclusively, to the use of fluoroscopy to acquire information during surgery and during placement of catheters, needles, and other devices.)
Within
the professions of radiology and radiologic physics,
there are mainstream experts who have shown how the dosage of
xrays in current practice could be cut by 50%, or by
considerably more, in diagnostic and interventional radiology
--- without any loss of information and without eliminating a
single procedure (discussion in Part 9,
below). Among the current leaders in dose-reduction education are
Joel Gray, Ph.D. (recently retired from the Mayo Clinic's Department of
Radiology in Rochester, Minnesota) and Fred Mettler, M.D. (Chief
of Radiology, University of New Mexico School of Medicine in
Albuquerque, New Mexico).
This monograph has produced evidence with regard to two hypotheses.
* Hypothesis-1: Medical radiation is a highly important cause (probably the principal cause) of cancer mortality in the United States during the Twentieth Century. Medical radiation means, primarily but not exclusively, exposure by xrays --- including fluoroscopy and CT scans. (Hypothesis-1 is about causation of Cancer, so it is silent about radiation-therapy used after a Cancer has been diagnosed.)
* Hypothesis-2: Medical radiation, received even at very low and moderate doses, is an important cause of death from Ischemic Heart Disease (IHD); the probable mechanism is radiation-induced mutations in the coronary arteries, resulting in dysfunctional clones (mini-tumors) of smooth muscle cells. (The kinds of damage to the heart and its vessels, observed from very high-dose radiation and reported for decades, seldom resemble the lesions of IHD --- details in Appendix J.)
4a. These
Hypotheses in Terms of Multi-Cause Diseases
Cancer and Ischemic Heart Disease are well established as multi-cause diseases. The concept, that more than one necessary co-actor is required per case, has already been discussed in Parts 4 and 5 of the Introduction. In efforts to prevent these multi-cause diseases, reduction or removal of any necessary co-actor is a central goal. The evidence in this book is that medical radiation has become a necessary co-actor in a high fraction of the U.S. mortality rates from both diseases. Fortunately, dosage from medical radiation is demonstrably reducible without eliminating a single procedure.
4b. Fractional
Causation: Percentage of Death-Rates due to Medical Radiation
The tabulation below shows the percentages, of the age-adjusted death rates (m=male, f=female) from Cancer and IHD, due to medical radiation at mid-century and at the most recent year for which we have data. Box 1 at the end of this chapter shows percentages for several specific types of Cancer. Percentages for each intervening decade are shown in the appropriate chapters and assembled in Chapter 66.
When an entry of ~ 100% occurs, such a finding is fully consistent with the fact that these diseases occurred before the introduction of radiation into medicine, over a century ago. Other mutagens (including radiation exposure from nature itself) have been operative both before and after the introduction of medical radiation. A finding, of about 100% of the death-rate due to medical radiation in 1940, means that by 1940, a very low fraction of such deaths would have occurred without medical radiation as a co-actor.
Year Percent Year Percent
* All-Cancers-Combined, m 1940 90% 1988 74%
* All-Cancers-Combined, f 1940 58% 1988 50%
* Breast Cancer, f 1940 ~ 100% 1990 83%
* All-Cancer-Except-Genital, f 1940 75% 1980 66%
* Ischemic Heart Disease, m 1950 79% 1993 63%
* Ischemic Heart Disease, f 1950 97% 1993 78%
The growing impact of cigarette smoking (Chapters 48, 49) almost certainly explains why the shares from medical radiation in 1980-1993 are somewhat lower than in 1940-1950.
A percentage such as 90% due to medical radiation (Fractional Causation by medical radiation = 0.90) means that about 90% of the death-rate would have been absent in the absence of medical radiation. Circumstantial evidence is strong that nonxray agents also were necessary co-actors in these same deaths. Thus, Fractional Causation of 90% by medical radiation certainly does not leave "just 10%" for all other causes combined, as already illustrated in Part 5 of the Introduction.
Fractional Causation, of a year-specific mortality rate (MortRate) by medical radiation, refers to whatever rate occurs in that year, and says nothing about whether the MortRate has been rising or falling over time. Indeed, changes over time, in the types and concentrations of non-xray co-actors to which populations are exposed, can cause cancer MortRates simultaneously to rise for some organs, fall for other organs, and remain constant for still other organs (discussion in Chapter 67, Part 2).
The
results in this book amply support Hypothesis-1 and the
first part of Hypothesis-2. While the central estimates of
Fractional Causation are statistically the most likely to be
correct, of course the actual percentages could be either higher
or lower. We note that percentages very much lower than the
central estimates would support each hypothesis, too.
When increments, in the death-rate from a disease, are proportional to increments in exposure to an identified cause, a linear dose-response exists between the causal agent and increments in the death-rate.
The
evidence in this monograph repeatedly reveals a positive and
tight linear dose-response, between dose from medical radiation
and mortality rates from Cancer (discussion in
Chapter 5,
Part 5d).
By "tight," we mean highly reliable (statistically). As
we will explain, no group in our database escapes entirely from
exposure to medical radiation. In order to estimate what the
cancer mortality rates would be in the absence of medical
radiation, we use the basic technique of linear regression
analysis (Part 5c, below). After that basic
step, it is not at all complicated to calculate Fractional
Causation due to medical radiation
(Part 5g, below).
We acquired the age-adjusted cancer MortRates per 100,000 population in each of the Nine Census Divisions of the USA, from 1940 onward --- separately for males and females, and for all races combined (no exclusions). Such data are published by the U.S. Government (details in Chapter 4). For most types of Cancer, our data end in 1988-1990 (some end in 1980).
Also we acquired the comparable age-adjusted MortRates for All NonCancer Causes of Death --- as well as for selected individual causes (such as IHD, Stroke, Diabetes Mellitus, Influenza and Pneumonia, Accidents, etc.) --- in each of the Nine Census Divisions.
These
MortRates, by Census Divisions, are the dependent
variables (the responses) in our dose-response studies. Because
the MortRates are age-adjusted, the Census Divisions are matched
with each other for age.
During the 1985-1990 period, the number of diagnostic medical xray examinations performed per year in the USA was approximately 200 million, excluding 100 million dental xray examinations and 6.8 million diagnostic nuclear medicine examinations. The source of these estimates (the 1993 Report of UNSCEAR, the United Nations Scientific Committee on Atomic Radiation, p.229, p.275) warns that 200 million could be an underestimate by up to sixty percent.
Not only is the number of annual examinations quite uncertain, but the average doses per examination --- in actual practice, not measured with a dummy during ideal practice --- vary sometimes by many-fold from one facility to another, even for patients of the same size. The variation by facility has been established by a few on-site surveys of selected facilities, because measurement and recording of xray doses are not required for actual procedures (Part 9, below).
Fluoroscopy is a major source of xray dosage, because the xray beam stays "on" during fluoroscopy. Such doses are rarely measured. When fluoroscopic xrays are used during common diagnostic examinations, the total dose delivered varies with the operator. When fluoroscopic xrays are used during surgery and other nondiagnostic procedures, the total dose delivered varies both with the operator and the particular circumstances.
The uncertain number of procedures and the very uncertain doses per procedure combine to cause profound uncertainty about current average per capita population dose from medical radiation (Chapter 2, Part 3). Dose estimates for past decades are even more uncertain (Chapter 2, Part 2).
An Additional Gap in Knowledge: Risk-per-Rad Estimates
In most of the studies which produce estimates of cancer-risk per rad of xray dose, it is far from certain which participants received which xray doses over their lifetimes, because such doses were neither measured nor recorded. When a few participants are (unintentionally) assigned a wrong dose-estimate, the error can substantially alter the resulting risk-per-rad estimates. This contributes to the great uncertainty about the true risk-per-rad from xrays (Chapter 2, Part 7c). The uncertainty is no secret. For example, the fifth Committee on the Biological Effects of Ionizing Radiation stated in its 1990 report (National Academy Press, at pp.46-47): "A number of low-dose studies have reported risks that are substantially in excess of those estimated in the present report ... Although such studies do not provide sufficient statistical precision to contribute to the risk estimation procedure per se, they do raise legitimate questions about the validity of the currently accepted estimates."
A Solution to These Gaps in Knowledge
Medical radiation procedures are initiated by a physician, even if someone else actually performs the procedure. It is very reasonable to think that the more physicians there are per 100,000 population, the more radiation procedures per 100,000 population will be ordered. Thus, we arrive at the premise that average radiation dose, received per capita of population in a specific Census Division from medical procedures during a specific year, is approximately proportional to the number of physicians per 100,000 population in that same Census Division during that same year.
This common-sense premise is well supported in the 1988 and 1993 reports of the United Nations Scientific Committee on Atomic Radiation (details in our Chapter 3, Part 1a), and is supported specifically for the USA by data in a 1989 report from the National Council on Radiation Protection and Measurements (details in Chapter 3, Part 1a).
"PhysPop" Values in the Nine Census Divisions, over Many Decades
We use the abbreviation, "PhysPop," for the quantity "Physicians per 100,000 Population." A PhysPop value of 134 means 134 Physicians per 100,000 population, for the specified year and place.
PhysPop values for various calendar years have been compiled and published for each state by the American Medical Association over many decades (details in Chapter 3). It is a routine matter to combine such data appropriately, in order to obtain PhysPop values for the Nine Census Divisions (details in Chapter 3). Because substantial differences in PhysPop values exist among the Nine Census Divisions, it has been possible for us to do dose-response studies, with PhysPop values in each Census Division as surrogates for average per capita dose from medical radiation in each corresponding Census Division.
Of
course, dose is cumulative (i.e., radiation-induced mutations
are cumulative). Moreover, in a population of mixed ages
(newborn to very advanced ages), the cancer-response to ionizing
radiation is spread out over at least four to five decades
(Chapter 2,
Part 8). Thus,
the age-adjusted cancer MortRates in
any single year --- say 1990 --- incorporate cases which are due
to radiation received in 1940, 1950, 1960, 1970, etc. It happens
that, during the 1921-1990 period, the rank order of the Census
Divisions --- by the size of their PhysPop values --- has been
remarkably stable (details in Chapter 3,
Box 1; see also Chapter
47, Table 47-A). Thus, PhysPop values are well-suited to be
surrogates for the relative size of average accumulated per
capita dose from medical radiation, among the Nine Census
Divisions.
Linear regression analysis is a branch of mathematics which, among other things, evaluates how well correlated are sets of paired values. In our dose-response studies, there are always nine pairs of values, because there are Nine Census Divisions --- each having its own age-adjusted MortRate (the y-variable) and its own PhysPop value (the x-variable). On the lefthand side of the next page, we show the input data for a regression whose output is shown on the righthand side.
In the output, two quantities measure the goodness (strength) of the correlation: The R-squared value, and the ratio of the X-coefficient divided by its Standard Error (X-Coef/S.E.).
* An R-squared value of 1.00 is perfection. An R-squared value of 0.70 is very good. Those who are familiar with the correlation coefficient, R, will recognize that R-squared values are lower than the corresponding R-values (for instance, when R = 0.83666, R-squared = 0.70; when R = 0.94868, R-squared = 0.90).
* A ratio of (X-Coef/S.E.) of about 2.0 generally indicates a statistically significant correlation. A ratio of 4.0 is a tight correlation. A ratio above 4.0 is very tight. The ratio describes the reliability of the slope in a line of best fit.
In
Part 5d, the male 1940 MortRates per 100,000 population, for
All-Cancers-Combined, are regressed upon the 1940 PhysPop values
(which represent accumulated doses from earlier years of medical
radiation). The regression reveals a spectacularly tight
correlation: R-squared = 0.9508.
Dose-Response (Males, Females)
The regression output (below) provides all the information necessary to calculate and to graph the line of best fit for the nine pairs of real-world observations (listed below). Chapter 6, Part 3, shows how. The resulting graph is presented in the upper half of Figure 1-A, at the end o this chapter. The nine boxy symbols in Figure 1-A represent the nine pairs of actual observations from the x,y columns below. For example, the box farthest to the right represents the pair with the highest PhysPop value: The Mid-Atlantic pair.